Kaiser Permanente nursing excellence: 75 years in the making
The founding principles and vision of nursing started in 1933. and paved the way for high-performing nurse specialties today.
Kaiser Permanente's first nurse, Betty Runyen, at Desert Center in 1933.
The history of nursing at Kaiser Permanente actually begins in 1933 with Betty Runyen, the sole permanent nurse of Sidney R. Garfield, MD, at the Desert Center Hospital near the construction site of the Los Angeles Aqueduct. Runyen, a young nursing graduate from Los Angeles, was just starting out and looking for adventure.
She was well aware of the early 20th century restrictions on her career options. Her mother had told her she could be a secretary, a teacher or a nurse. Nursing sounded the most intriguing. She became bored with her first job helping to birth babies, and sprung at the opportunity to help launch this pioneering hospital in the desert.
In 1933 nurses were not expected, or even allowed, to perform such a task as starting an IV (tube to introduce liquid intravenously). But Garfield, co-founder of Kaiser Permanente with Henry J. Kaiser, was forward thinking. He had taught Runyen how to start an IV, and the skill came in handy one day when she received an emergency call that one of the workers had succumbed to heat exhaustion. Dr. Garfield was not around, so she drove the ambulance to the job site and immediately inserted a saline IV. The patient quickly recovered.
Looking back from 2011, it seems absurd that nurses — usually women — weren’t entrusted with a task that is now considered routine. But this fact is indicative of how far nurses have come in 75 years in America and at Kaiser Permanente. A review of Kaiser Permanente’s history reflects the major strides the nursing community has made, bringing them to a place and time where their skills are as varied and as specialized and expert as physicians.
Kaiser Permanente's history reflects national trends
Nursing history is also punctuated with challenges related to the nurse’s evolving role on the medical care team and with major changes in technology, including medical equipment and the use of computers to record medical notes.
In the 1960s, 1970s, and 1980s, care of patients shifted away from the hospital to outpatient settings. Advances in technology made it possible for surgery patients to spend less time in the hospital, and Medicare reimbursement policy, revised in 1983 dictated shorter hospital stays. Despite a growing and aging population, the length of stay national average trended down from 8.5 days in 1968 to 6.4 days in 1990 to 4.8 days in 2005, according to the Centers for Disease Control.
Wartime Oakland nurses confer with pioneer KP physician Cecil Cutting.
These changes spawned the same day surgery program that allowed patients to have a procedure without staying overnight. The Kaiser Permanente home care program was beefed up to provide surgery and hospitalization follow-up. Outpatient chronic condition management — for the benefit of the patient and the health plan — became ever more important to minimize the time patients had to spend in the hospital. Changes in maternity care also led to shorter hospital stays and an emphasis on family-centered perinatal practices.
New nursing specialties emerge
New categories of nursing have popped up throughout the decades. In the 1970s, the nurse practitioner role was developed to perform many of the tasks formerly done by physicians. For example, the KP multiphasic or annual physical, initiated in the 1950s for the longshoremen’s union and expanded to the general membership, began to be administered by nurse practitioners working under the supervision of physicians. Nurse practitioners were also tapped for well baby care and routine pediatrics visits as medical roles morphed during a critical shortage of medical manpower in America.
With Kaiser Permanente’s emphasis on preventive care, its nurses have been called on to create outpatient education programs to help members manage their own health in partnership with their medical care team. Nurses have become specialized in outpatient management of chronic conditions such as heart disease and diabetes, and in providing home and hospice care. Specialized nursing roles have multiplied exponentially over the decades with today’s nurses trained in every aspect of medicine: surgery, intensive care, cardiac care, obstetrics, geriatrics, orthopedics, and the list goes on.
-
Social Share
- Share Kaiser Permanente Nursing Excellence: 75 Years in the Making on Pinterest
- Share Kaiser Permanente Nursing Excellence: 75 Years in the Making on LinkedIn
- Share Kaiser Permanente Nursing Excellence: 75 Years in the Making on Twitter
- Share Kaiser Permanente Nursing Excellence: 75 Years in the Making on Facebook
- Print Kaiser Permanente Nursing Excellence: 75 Years in the Making
- Email Kaiser Permanente Nursing Excellence: 75 Years in the Making

July 16, 2025
A new gold standard in nursing excellence
Woodland Hills Medical Center is our first hospital in Southern California …
April 30, 2025
A history of trailblazing nurses
Nursing pioneers lay the foundation for the future of Kaiser Permanente …

April 30, 2025
Celebrate National Nurses Week with me
Join us in honoring our nurses for their dedication to providing high-quality, …

April 30, 2025
Celebrating our extraordinary nurses
Our nurses are leaders and patient advocates. They transform care and improve …

April 16, 2025
Sidney R. Garfield, MD: Pioneer of modern health care
Kaiser Permanente’s co-founding physician spread prepaid care and the idea …

February 24, 2025
Honoring extraordinary nurses
Our award-winning nurses put patients first and contribute new knowledge …

September 19, 2024
First look at new Lakewood facilities
New medical offices will enhance the health care experience for members …

May 3, 2024
Henry J. Kaiser: America’s health care visionary
Kaiser was a major figure in the construction, engineering, and shipbuilding …

April 9, 2024
Building partnerships to inspire the next generation
Kaiser Permanente supports education and career opportunities for students …

April 8, 2024
Martin Luther King Jr.’s dream is alive at Kaiser Permanente
Greg A. Adams, chair and chief executive officer of Kaiser Permanente, …

February 13, 2024
A legacy of life-changing community support and partnership
The Kaiser Permanente Watts Counseling and Learning Center started as a …

February 2, 2024
Expanding medical, social, and educational services in Watts
Kaiser Permanente opens medical offices and a new home for the Watts Counseling …

October 17, 2023
How Kaiser Permanente evolved
Sidney R. Garfield, MD, and Henry J. Kaiser came together to pioneer an …

October 3, 2023
Nursing excellence recognized at Fontana Medical Center
The prestigious Magnet® designation affirms the compassion, dedication, …

September 13, 2023
Transforming the medical record
Kaiser Permanente’s adoption of disruptive technology in the 1970s sparked …

August 8, 2023
Nursing excellence: Joining the elite 10% in the nation
Kaiser Permanente Panorama City Medical Center achieves coveted Magnet® …

May 18, 2023
The gold standard of nursing excellence
Kaiser Permanente Baldwin Park Medical Center achieves Magnet status, the …

May 2, 2023
Women lead an industrial revolution at the Kaiser Shipyards
Early women workers at the Kaiser shipyards diversified home front World …

April 25, 2023
Hannah Peters, MD, provides essential care to ‘Rosies’
When thousands of women industrial workers, often called “Rosies,” joined …

November 11, 2022
A history of leading the way
For over 75 innovative years, we have delivered high-quality and affordable …
November 11, 2022
Pioneers and groundbreakers
Learn about the trailblazers from Kaiser Permanente who shaped our legacy …
November 11, 2022
Our integrated care model
We’re different than other health plans, and that’s how we think health …
November 11, 2022
Our history
Kaiser Permanente’s groundbreaking integrated care model has evolved through …
October 14, 2022
Contact Heritage Resources

October 6, 2022
We’re a Fast Company Innovation by Design winner
Kaiser Permanente is the first health care organization to win Design Company …
October 1, 2022
Innovation and research
Learn about our rich legacy of scientific research that spurred revolutionary …

May 26, 2022
Nurse practitioners: Historical advances in nursing
A doctor shortage in the late 1960s and an innovative partnership helped …
September 10, 2021
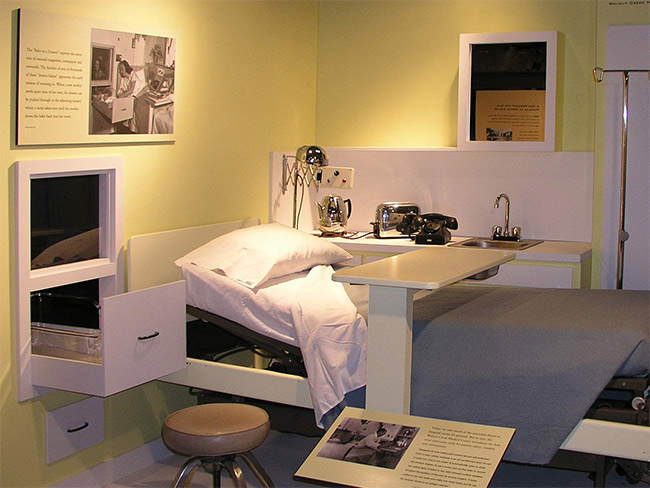
‘Baby in the drawer’ helped turn the tide for breastfeeding
This innovation in rooming-in allowed newborns to stay close to mothers …

August 25, 2021
Kaiser Permanente’s history of nondiscrimination
Our principles of diversity and our inclusive care began during World War …

July 22, 2021
A long history of equity for workers with disabilities
In Henry J. Kaiser’s shipyards, workers were judged by their abilities, …

June 2, 2021
Path to employment: Black workers in Kaiser shipyards
Kaiser Permanente, Henry J. Kaiser’s sole remaining institutional legacy, …

February 22, 2021
The Permanente Richmond Field Hospital
Forlorn and all but forgotten, it played a proud role during the World …

September 28, 2020
A legacy of disruptive innovation
Proceeds from a new book detailing the history of the Kaiser Foundation …

August 26, 2020
Kaiser Permanente’s pioneering nurse-midwives
The 1970s nurse-midwife movement transformed delivery practices.

July 30, 2020
Books and publications about our history
Interested in learning more about the history of Kaiser Permanente and …

May 18, 2020
Nurses step up in crises
Kaiser Permanente nurses have been saving lives on the front lines since …

November 8, 2019
Swords into stethoscopes — veterans in health professions
Kaiser Permanente has actively hired veterans in all capacities since World …

August 28, 2019
When labor and management work side by side
From war-era labor-management committees to today’s unit-based teams, cooperation …

August 2, 2019
Thriving with 1960s-launched KFOG radio
Kaiser Broadcasting radio connected listeners, while TV stations brought …

June 5, 2019
Breaking LGBT barriers for Kaiser Permanente employees
“We managed to ultimately break through that barrier.” — Kaiser Permanente …

March 29, 2019
Equal pay for equal work
Kaiser shipyards in Oregon hired the first 2 female welders at equal pay …

February 5, 2019
Mobile clinics: 'Health on wheels'
Kaiser Permanente mobile health vehicles brought care to people, closing …

December 10, 2018
Southern comfort — Dr. Gaston and The Southeast Permanente Medical Group
Local Atlanta physicians built community relationships to start Kaiser …

May 30, 2018
John Graham Smillie, MD, pediatrician and innovator
Celebrating the life of a pioneering pediatrician who inspired the baby …

April 30, 2018
Nursing pioneers leads to a legacy of leadership
Kaiser Foundation School of Nursing students learned a new philosophy emphasizing …

April 19, 2018
Wasting nothing: Recycling then and now
Environmentalism was a common practice at the Kaiser shipyards long before …

April 12, 2018
Harold Hatch, health insurance visionary
The founding of Kaiser Permanente's concept of prepaid health care in the …

March 26, 2018
5 physicians who made a difference
Meet 5 outstanding doctors who advanced the practice of medical care with …

March 13, 2018
Henry J. Kaiser and the new economics of medical care
Kaiser Permanente’s co-founder talks about the importance of building hospitals …

March 8, 2018
Slacks, not slackers — women’s role in winning World War II
Women who worked in the Kaiser shipyards helped lay the groundwork for …

February 22, 2018
The amazing true story of Park Ranger Betty Reid Soskin
She is the oldest national park ranger in the country with a legacy of …

December 19, 2017
From boats to books: A history of Kaiser Permanente’s medical libraries
Kaiser Permanente librarians are vital in helping clinicians remain updated …

November 7, 2017
Patriot in pinstripes: Honoring veterans, home front, and peace
Henry J. Kaiser's commitment to the diverse workforce on the home front …

October 12, 2017
An experiment named Fabiola
Health care takes root in Oakland, California.

September 29, 2017
Harbor City Hospital: Beachhead for labor health care
The story of Kaiser Permanente's South Bay Medical Center finds its roots …

August 15, 2017
Sidney R. Garfield, MD, on medical care as a right
Hear Kaiser Permanente’s physician co-founder talk about what he learned …

August 10, 2017
‘Good medicine brought within reach of all'
Paul de Kruif, microbiologist and writer, provides early accounts of Kaiser …

July 14, 2017
Kaiser’s role in building an accessible transit system
Harold Willson, an employee, and an advocate for accessible transportation, …

July 7, 2017
Mending bodies and minds — Kabat-Kaiser Vallejo
The expanded new location provided care to a greater population of members …

June 23, 2017
No getting round it: An innovative approach to building design
Kaiser Permanente incorporated innovative circular architectural designs …

June 14, 2017
Kabat-Kaiser: Improving quality of life through rehabilitation
When polio epidemics erupted, pioneering treatments by Dr. Herman Kabat …
June 9, 2017
Edmund (Ted) Van Brunt, pioneer of electronic health records, dies at age …
Throughout his career, Dr. Van Brunt applied computers and databases in …

May 4, 2017
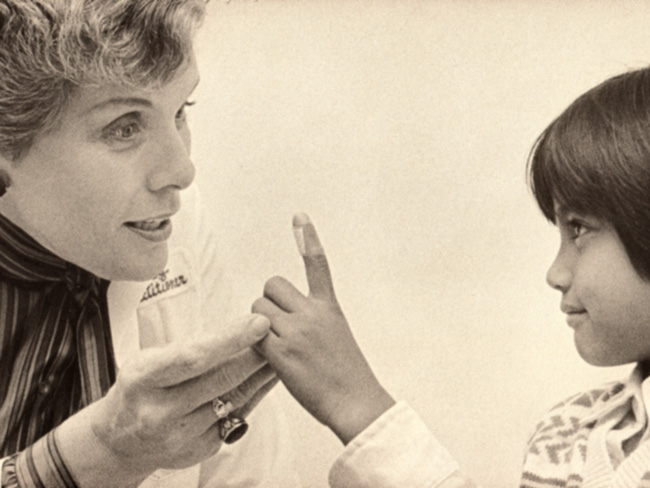
How a Kaiser Permanente nurse transformed health education
Kaiser Permanente's Health Education Research Center and Health Education …
March 22, 2017
Kaiser Permanente and Group Health Cooperative: Working together since …
The formation of Kaiser Permanente Washington comes from longstanding collaboration, …

March 7, 2017
Beatrice Lei, MD: From Shantou, China, to Richmond, California
She served as a role model and inspiration to the women physicians and …
March 1, 2017
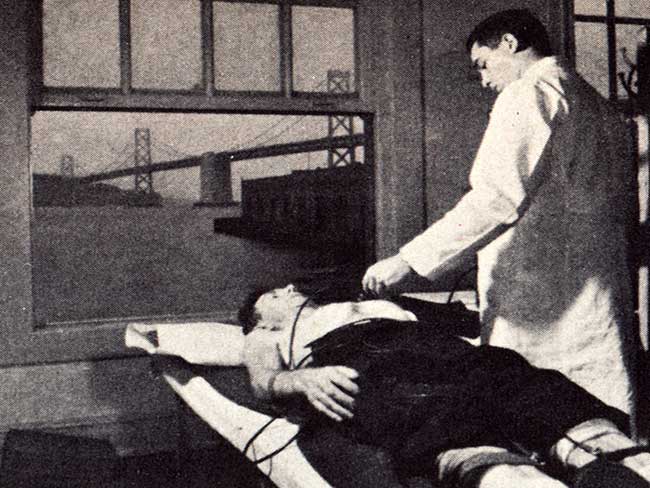
Screening for better health: Medical care as a right
When industrial workers joined the health plan, an integrated battery of …
February 17, 2017
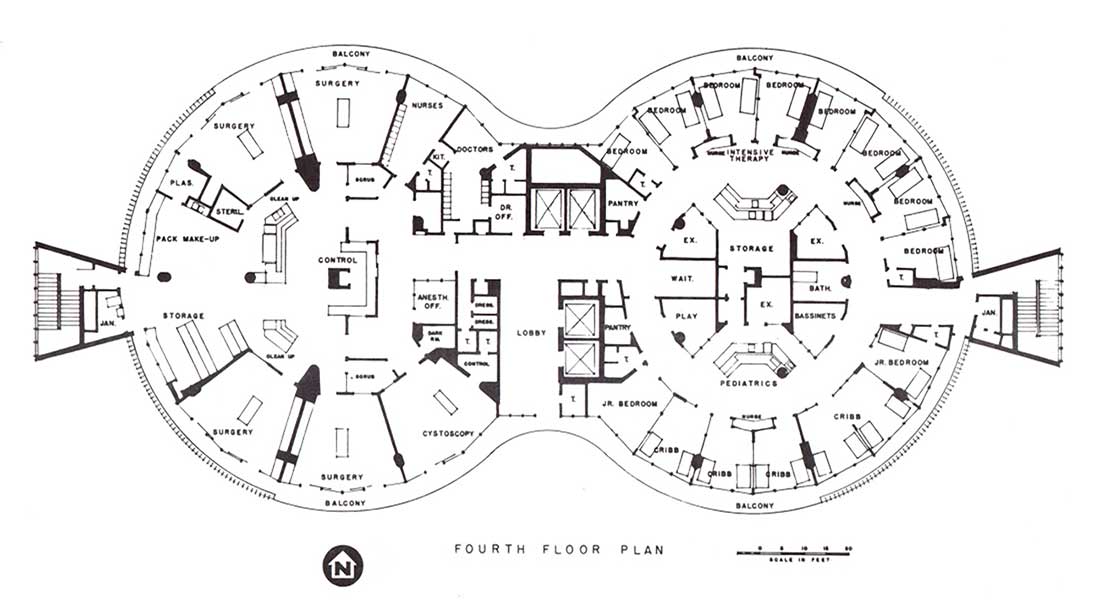
Experiments in radial hospital design
The 1960s represented a bold step in medical office architecture around …

February 3, 2017
Ellamae Simmons — trailblazing African American physician
Ellamae Simmons, MD, worked at Kaiser Permanente for 25 years, and to this …

January 27, 2017
Japanese-American doctors overcame internment setbacks
Despite restrictive hiring practices after World War II, Kaiser Permanente …

November 16, 2016
Betty Reid Soskin honored with lifetime achievement award
The California Studies Association presents the Carey McWilliams Award …

October 17, 2016
Kaiser Motors in Oakland — “We sell to make friends.”
In 1946 Henry J. Kaiser Motors purchased half a square block in downtown …
October 12, 2016
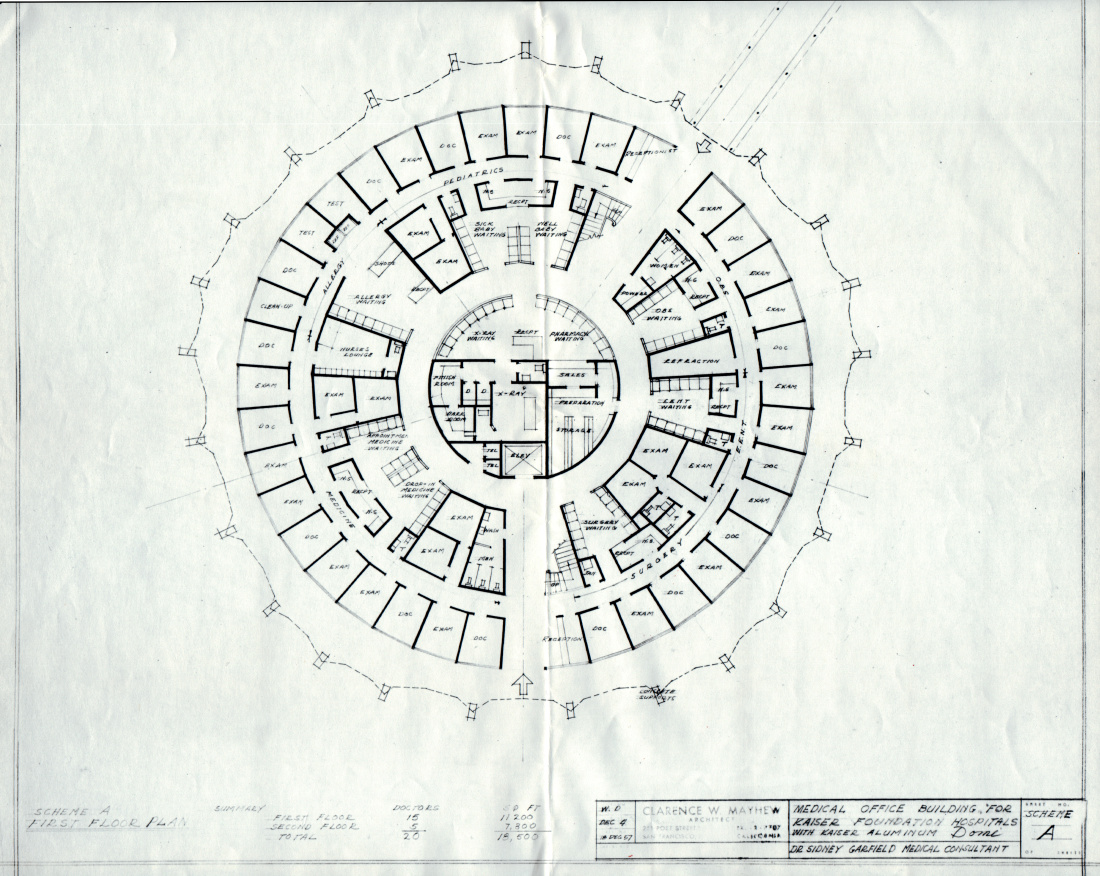
Kaiser’s geodesic dome clinic
There are hospital rounds, and there are round hospitals.

May 5, 2016
Male nursing pioneers
Groundbreaking male students diversify the Kaiser Foundation School of …
April 20, 2016
Henry J. Kaiser’s environmental stewardship
Since the 1940s, Kaiser Industries and Kaiser Permanente have a long history …

November 13, 2015
Dr. Morris Collen’s last book on medical informatics
The last published work of Morris F. Collen, MD, one of Kaiser Permanente’s …

October 29, 2015
From paper to pixels — the new paradigm of electronic medical records
Transitioning to electronic health records introduced new approaches, skills, …

September 23, 2015
Kaiser Permanente and NASA — taking telemedicine out of this world
Kaiser Permanente International designs, develop, and test a remote health …

July 22, 2015
Kaiser Permanente as a national model for care
Kaiser Permanente proposed a revolutionary national health care model after …

July 21, 2015
Kaiser Permanente's early support from labor
Experiencing the Kaiser Permanente health plan led labor unions to support …

July 20, 2015
Opening the Permanente plan to the public
On July 21, 1945, Henry J. Kaiser and Dr. Sidney Garfield offered the health …

July 1, 2015
Sculpture dedicated to Kaiser Nursing School
The Kaiser Foundation School of Nursing sculpture near Kaiser Oakland hospital …

May 6, 2015
Celebrating Betty Runyen — Kaiser Permanente’s ‘founding nurse’
In a desert hospital during the Great Depression, Betty Runyen overcame …
April 27, 2015
Eugene Hickman, MD — Pioneering Black physician
Dr. Hickman had a long career at Kaiser Permanente, becoming president …

April 24, 2015
2 historical reflections on Kaiser Permanente

April 2, 2015
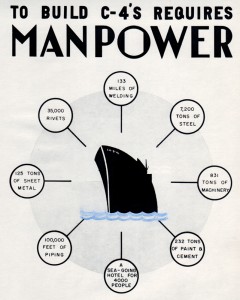
Henry Kaiser’s escort carriers and the Battle of Leyte Gulf
January 9, 2015
The World War II Kaiser Richmond shipyard labor force

December 16, 2014
Henry J. Kaiser on veteran employment and benefits

December 11, 2014
Henry J. Kaiser, geodesic dome pioneer
July 23, 2014
Kaiser shipyards pioneered use of wonder drug penicillin
Though supplies for civilians were limited, Dr. Morris Collen’s wartime …

June 24, 2014
Kaiser Permanente's first hospital changes and grows
A collection of vintage photos that chronicle the evolution of Oakland …

June 20, 2014
Old hospital holds memories of Kaiser Permanente’s past
Rebuilt Oakland Medical Center to open for business.

May 13, 2014
Henry J. Kaiser sticks up for union labor at Brewster Aeronautical

May 5, 2014
Black nurses get together to forge their own future
California African American nurses organize in early 1970s to address health …

May 1, 2014
Beloved nurse earned place in Kaiser Permanente history
Jessie Cunningham, the first Black nursing supervisor at Oakland Medical …

February 18, 2014
Alva Wheatley: Champion of Kaiser Permanente diversity
Third in a series marking Black History Month.

January 31, 2014
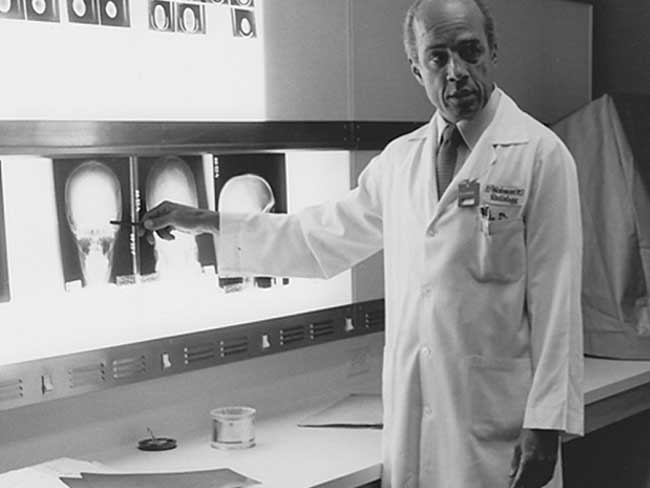
Raleigh Bledsoe, MD: First Black radiologist west of Rockies
Dr. Bledsoe became the first Black physician for Southern California Permanente …

January 23, 2014
Kaiser's first labor attorney in the thick of union battles
Harry F. Morton was an instrumental figure at Henry J. Kaiser's side, setting …

October 16, 2013
Georgia cardiologist returns to Atlanta to start new Permanente group
Kaiser Permanente expands to the Southeast and builds community relations …

October 8, 2013
Northwest Region started small and grew fast
Kaiser Permanente remained and opened the Northwest Region after World …

October 7, 2013
The roots of Southern California Kaiser Permanente
Kaiser Permanente Southern California started from its roots at the Fontana …