Research transforms care for people with multiple sclerosis
Our researchers are leading the way to more effective, affordable, and equitable care.
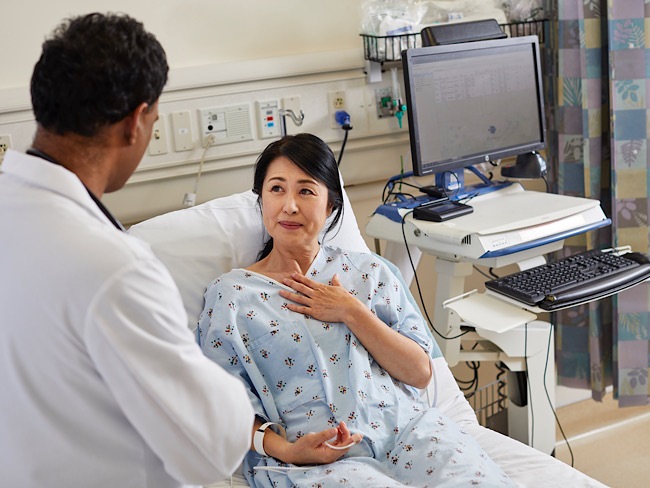
Annette Langer-Gould, MD, PhD, studies treatments to improve care for people with MS. Jacques Roussel is a patient partner in one of her studies.
Treatment for multiple sclerosis needs to change. At Kaiser Permanente, it already has.
We’ve improved care thanks to research conducted by Annette Langer-Gould, MD, PhD, and her colleagues.
Dr. Langer-Gould wants the rest of the world to follow. She co-authored an article in the journal Neurology urging the medical community to adopt use of a medication that has the potential to improve care for many patients.
Dr. Langer-Gould, a neurologist and a scientist who studies MS, discusses what she’s learned through her research.
What is MS?
MS is a disease that affects the brain and spinal cord, often leading to permanent disability. It cannot be cured. But medications can help reduce the risk of disability.
Nearly a million people in the United States have MS. For most people, the disease starts with a rather sudden onset of symptoms. Those symptoms may go away or lessen with time. If new symptoms appear or old symptoms return for a period of time, it’s called a relapse.
Why does MS treatment need to change?
People with more aggressive MS benefit from stronger drugs. However, in the United States, many people can’t afford the copays. Sometimes people don’t get the treatment they need and become disabled.
At Kaiser Permanente in Southern California, our Multiple Sclerosis Treatment Optimization Program ensures that more people with relapsing MS receive highly effective drugs as early in the disease course as possible.
Key to the program is our increased use of a drug called rituximab. This drug is more traditionally used for cancer and other diseases. But evidence shows it’s safe and highly effective for relapsing MS. And it costs much less than other options.
Many insurance carriers in the United States and Europe limit coverage of rituximab for treating MS. They’ve cited a lack of regulatory approval for use of the drug to treat MS. But that may be changing.
The World Health Organization now lists rituximab as an essential drug for MS. I hope other organizations will follow. Wider use could have significant benefits for patients and could reduce inequities.
How has your research led you to push for a shift?
A study we published in 2022 found that MS relapse rates plummeted for Kaiser Permanente members in Southern California during the initial rollout of our program. Thanks in part to the lower cost of rituximab, the cost of treatment has fallen.
And patients say they love rituximab. Besides being effective and affordable, it’s long-lasting, so they don’t need to come to the office as often. That means more people tend to stick with treatment over time.
What’s more, research in Sweden showed similar benefits of rituximab for patients. The country’s health care system has now approved it for MS. It really seems to be a game changer.
What drew you to study MS?
I began seeing MS patients as a medical resident and PhD student. It’s a chronic disease, so it gave me an opportunity to build rewarding, long-term relationships with patients. I also realized studying MS would be a chance to fight for underserved patients.
Our success with MS highlights Kaiser Permanente’s use of evidence-based medicine. We’re improving care based on evidence gathered through our research. And we hope the rest of the country follows our lead.
-
Social Share
- Share Research Transforms Care for People With Multiple Sclerosis on Pinterest
- Share Research Transforms Care for People With Multiple Sclerosis on LinkedIn
- Share Research Transforms Care for People With Multiple Sclerosis on Twitter
- Share Research Transforms Care for People With Multiple Sclerosis on Facebook
- Print Research Transforms Care for People With Multiple Sclerosis
- Email Research Transforms Care for People With Multiple Sclerosis

February 18, 2026
A better approach to preventing chronic conditions
With the right support from our policy leaders, we can help ensure fewer …

October 28, 2025
California employers, meet our smarter Choice plan
Kaiser Permanente Plus™ more affordably adds some out-of-network flexibility …

August 13, 2025
Celebrating 80: Kenneth Barnhart shares why he’s a member
As we celebrate our 80th anniversary, one member describes the high-quality, …

July 23, 2025
Celebrating 80: Cathy Hays shares why she’s a member
As we celebrate our 80th anniversary, one member describes the high-quality …

March 25, 2025
AI in health care: 7 principles of responsible use
These guidelines ensure we use artificial intelligence tools that are safe …

February 20, 2025
Kaiser Permanente joins Food Is Medicine Colorado coalition
As an inaugural member, Kaiser Permanente will help lead health care’s …

September 19, 2024
First look at new Lakewood facilities
New medical offices will enhance the health care experience for members …

July 10, 2024
Grant to help make school lunches healthier for kids
Chef Ann Foundation will use $275,000 grant for Colorado program to convert …

July 2, 2024
Reducing cultural barriers to food security
To reduce barriers, Food Bank of the Rockies’ Culturally Responsive Food …

June 28, 2024
Operation Splash makes a splash for safe summer fun
Kaiser Permanente is making waves this summer, ensuring that communities …

June 28, 2024
Health Action Summit highlights mental health opportunities
The Kaiser Permanente Colorado Health Action Summit gathered nonprofits, …

June 3, 2024
A call to ‘Connect’ for cancer prevention research
Participate in a study to help uncover the causes of cancer and how to …
April 23, 2024
We’re rising up to help prevent falls
Kaiser Permanente is committed to finding ways to help reduce falls in …

March 19, 2024
Fostering responsible AI in health care
With the right policies and partnerships, artificial intelligence can lead …

January 31, 2024
Prioritizing policies for health and well-being in Colorado
CityHealth’s 2023 Annual Policy Assessment awards cities for their policies …

December 6, 2023
Leaders named among health care’s most influential
Greg A. Adams; Maria Ansari, MD, FACC; and Ramin Davidoff, MD, have been …

December 6, 2023
Leading research with gratitude
Learn how you can participate in a study to uncover what causes cancer …

October 23, 2023
The future of health care is digital
Nari Gopala, Kaiser Permanente’s chief digital officer, answers 3 questions …

October 4, 2023
An easier way to manage multiple prescriptions
If you have an ongoing health condition, you know it can be tricky to keep …

September 27, 2023
10 school districts receive next round of RISE grants
The Thriving Schools program helps educators and students in Colorado integrate …

September 13, 2023
Transforming the medical record
Kaiser Permanente’s adoption of disruptive technology in the 1970s sparked …

April 25, 2023
Hannah Peters, MD, provides essential care to ‘Rosies’
When thousands of women industrial workers, often called “Rosies,” joined …
November 11, 2022
Our integrated care model
We’re different than other health plans, and that’s how we think health …

October 6, 2022
We’re a Fast Company Innovation by Design winner
Kaiser Permanente is the first health care organization to win Design Company …
October 1, 2022
Innovation and research
Learn about our rich legacy of scientific research that spurred revolutionary …
September 10, 2021
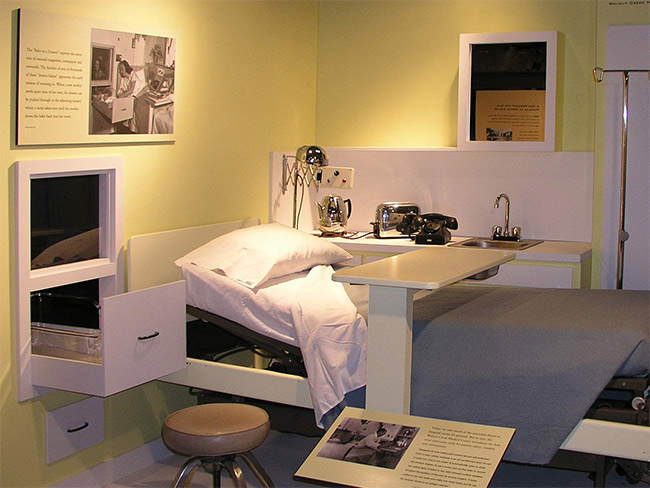
‘Baby in the drawer’ helped turn the tide for breastfeeding
This innovation in rooming-in allowed newborns to stay close to mothers …

February 22, 2021
The Permanente Richmond Field Hospital
Forlorn and all but forgotten, it played a proud role during the World …

September 28, 2020
A legacy of disruptive innovation
Proceeds from a new book detailing the history of the Kaiser Foundation …

August 26, 2020
Kaiser Permanente’s pioneering nurse-midwives
The 1970s nurse-midwife movement transformed delivery practices.

August 2, 2019
Thriving with 1960s-launched KFOG radio
Kaiser Broadcasting radio connected listeners, while TV stations brought …

February 5, 2019
Mobile clinics: 'Health on wheels'
Kaiser Permanente mobile health vehicles brought care to people, closing …

April 30, 2018
Nursing pioneers leads to a legacy of leadership
Kaiser Foundation School of Nursing students learned a new philosophy emphasizing …

April 19, 2018
Wasting nothing: Recycling then and now
Environmentalism was a common practice at the Kaiser shipyards long before …

April 12, 2018
Harold Hatch, health insurance visionary
The founding of Kaiser Permanente's concept of prepaid health care in the …

March 26, 2018
5 physicians who made a difference
Meet 5 outstanding doctors who advanced the practice of medical care with …

December 19, 2017
From boats to books: A history of Kaiser Permanente’s medical libraries
Kaiser Permanente librarians are vital in helping clinicians remain updated …

October 12, 2017
An experiment named Fabiola
Health care takes root in Oakland, California.

August 15, 2017
Sidney R. Garfield, MD, on medical care as a right
Hear Kaiser Permanente’s physician co-founder talk about what he learned …

August 10, 2017
‘Good medicine brought within reach of all'
Paul de Kruif, microbiologist and writer, provides early accounts of Kaiser …

July 14, 2017
Kaiser’s role in building an accessible transit system
Harold Willson, an employee, and an advocate for accessible transportation, …

July 7, 2017
Mending bodies and minds — Kabat-Kaiser Vallejo
The expanded new location provided care to a greater population of members …

June 23, 2017
No getting round it: An innovative approach to building design
Kaiser Permanente incorporated innovative circular architectural designs …

June 14, 2017
Kabat-Kaiser: Improving quality of life through rehabilitation
When polio epidemics erupted, pioneering treatments by Dr. Herman Kabat …
June 9, 2017
Edmund (Ted) Van Brunt, pioneer of electronic health records, dies at age …
Throughout his career, Dr. Van Brunt applied computers and databases in …

May 4, 2017
How a Kaiser Permanente nurse transformed health education
Kaiser Permanente's Health Education Research Center and Health Education …
March 1, 2017
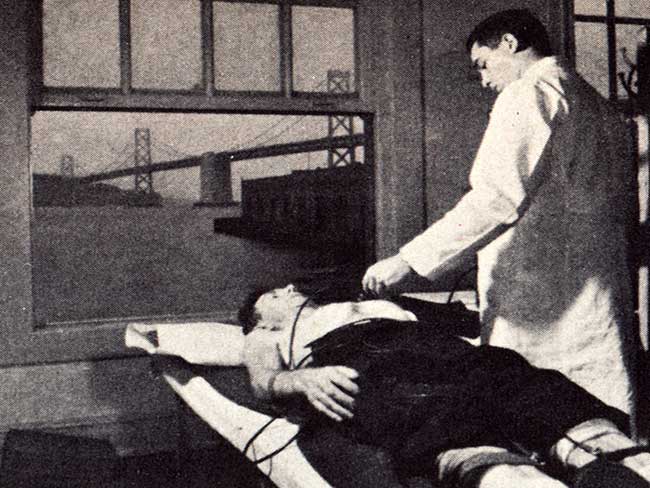
Screening for better health: Medical care as a right
When industrial workers joined the health plan, an integrated battery of …
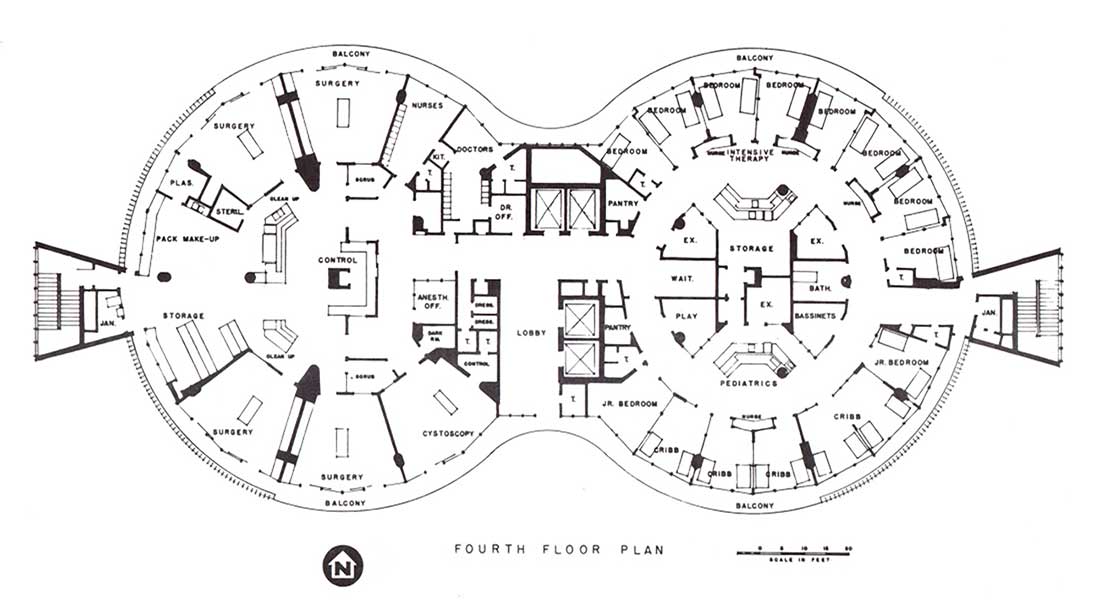
February 17, 2017
Experiments in radial hospital design
The 1960s represented a bold step in medical office architecture around …
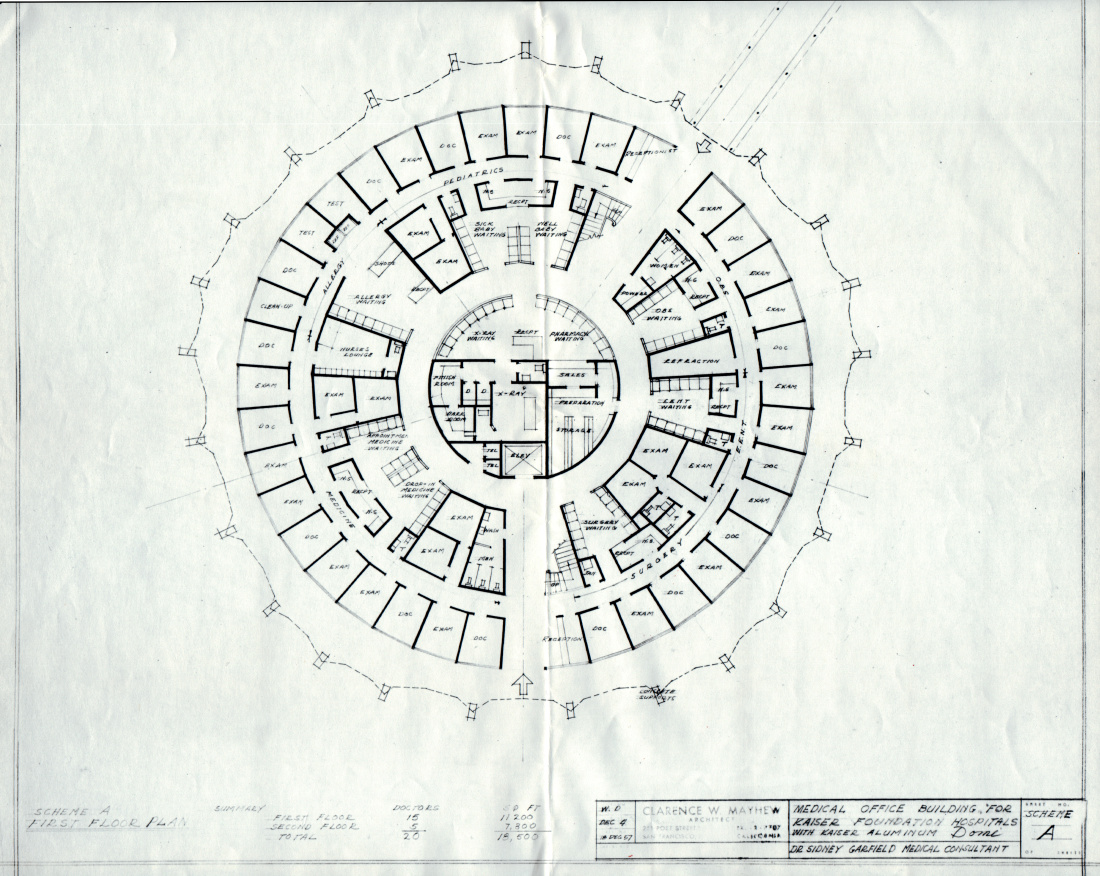
October 12, 2016
Kaiser’s geodesic dome clinic
There are hospital rounds, and there are round hospitals.
April 20, 2016
Henry J. Kaiser’s environmental stewardship
Since the 1940s, Kaiser Industries and Kaiser Permanente have a long history …

November 13, 2015
Dr. Morris Collen’s last book on medical informatics
The last published work of Morris F. Collen, MD, one of Kaiser Permanente’s …

October 29, 2015
From paper to pixels — the new paradigm of electronic medical records
Transitioning to electronic health records introduced new approaches, skills, …

September 23, 2015
Kaiser Permanente and NASA — taking telemedicine out of this world
Kaiser Permanente International designs, develop, and test a remote health …

July 22, 2015
Kaiser Permanente as a national model for care
Kaiser Permanente proposed a revolutionary national health care model after …

December 11, 2014
Henry J. Kaiser, geodesic dome pioneer

October 8, 2014
Breast cancer isn’t just a woman’s issue
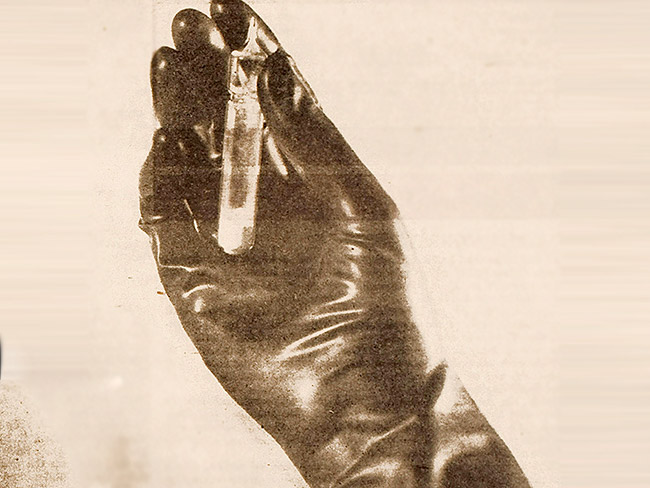
July 23, 2014
Kaiser shipyards pioneered use of wonder drug penicillin
Though supplies for civilians were limited, Dr. Morris Collen’s wartime …

June 24, 2014
Kaiser Permanente's first hospital changes and grows
A collection of vintage photos that chronicle the evolution of Oakland …

September 23, 2013
Kaiser Permanente pioneered solar power in health facilities in 1980
Santa Clara Medical Center hosted a solar panel project in 1979 to demonstrate …

September 19, 2013
Kaiser’s postwar suburbs designed for pedestrian safety and fitness
Model neighborhoods close to jobs and laid out with meandering lanes and …

July 9, 2013
Kaiser Permanente Web presence rooted in past
The first Kaiser Permanente website launched in 1996, creating a new way …

March 6, 2013
Decades of health records fuel Kaiser Permanente research
Over 50 years of early Kaiser Permanente electronic health records since …

October 23, 2012
Disabled Kaiser Permanente employee changed course of public transportation
In the 1960s, Harold Willson successfully advocated for the historically …

August 13, 2012
Marking half a century of stellar research
Kaiser Permanente's Division of Research has conducted pioneering health …

July 27, 2012
Millie Cutting: physician’s wife makes her own mark
From coordinating community groups to the World War II home front, Millie …

June 25, 2012
Early Permanente physician leader views health care future from 1966 vantage
Dr. Cecil Cutting, executive director of The Permanente Medical Group from …

March 14, 2012
Permanente pioneers step out to blaze their own quality trail
Dr. Leonard Rubin and Sam Sapin pioneered and piloted new quality assessment …

March 7, 2012
Permanente physicians strive to prove high quality of care
Early nation-wide health care quality assessments and evaluations became …
February 29, 2012
Quality of care: always foremost in minds of Kaiser Permanente leaders
Kaiser Permanente doctors applied research and innovation to implement …

August 8, 2011
Henry Kaiser among highway safety pioneers
Kaiser-Frazer automobiles pioneered and embraced safety engineering designs …

November 14, 2010
Kaiser-built 1954 sports car delights today’s collectors
Henry J. Kaiser and Howard Darrin collaborated on producing and designing …

October 20, 2010
Our long-standing commitment to sustainability
Kaiser Permanente invited Rachel Carson to speak after she published "Silent …