Lawmakers must act to boost telehealth and digital equity
Making key pandemic-era telehealth policies permanent and ensuring more people have reliable internet access will improve health outcomes for all.
By Cecilia Oregón, Executive Director, Kaiser Permanente Institute for Health Policy
Once considered a luxury, high-speed internet is now a necessity. People need reliable online access to connect to essential resources, including employment, education, finances, and — increasingly — health care.
And yet, not everyone has the ability or wherewithal to get online. This is a high-tech amplification of the inequality that has troubled America throughout its history. As our nation expands its reliance on the internet to access health care, as well as social and economic resources, this digital divide can lead directly to inequality in health outcomes.
To prevent this, we need public policies that aim for digital equity: Everyone should have the access, tools, and knowledge they need to get online. We also need policies that ensure everyone who wants and needs it can access virtual health care.
Pandemic-era policy makes telehealth more accessible
During the COVID-19 pandemic, an unprecedented number of people in the U.S. have received routine care away from traditional settings. For example, Kaiser Permanente, which was at the forefront of building virtual care capacity prior to the pandemic, delivered over 28 million telehealth visits in 2021 as our members sought care while staying safe at home. After an initial peak in 2020, telehealth use in 2021 settled at a level 38 times higher than before the pandemic, according to consulting firm McKinsey & Company.
Increased adoption of telehealth has resulted from strong demand, favorable consumer perception, and public and private investments. Congressional action also helped drive increases, allowing the Centers for Medicare & Medicaid Services to remove geographic restrictions so more patients could have virtual visits. CMS also increased the types of services Medicare covers and ensured more providers were eligible to offer telehealth to their patients.
Importantly, CMS also began covering phone-based visits for Medicare beneficiaries. This change was key to expanding access for many people, especially Black and Latino populations who often face “digital redlining,” when internet companies underinvest in providing service to communities that have lower incomes, resulting in lower-quality, less affordable broadband services.
State-level policymakers also have taken steps to increase telehealth adoption. They helped ensure Medicaid coverage for phone-based care and developed multistate licensure agreements, allowing people to access a wider variety of providers across state lines.
Challenges ahead
In late 2022, Congress extended policies, but many expire after 2024. State-level policymakers also must determine the next steps.
Meanwhile, increasing access to high-speed internet continues to be a challenge for our nation. People living in rural areas and those who have lower incomes, in both rural and urban areas, remain less likely to have home broadband or own a smartphone, tablet, or computer.
The billions of dollars for broadband expansion Congress passed in the Infrastructure Investment and Jobs Act was a promising step but also just the beginning.
Policymakers must take further action
To ensure continued access to telehealth, Congress should make key pandemic-era telehealth policies permanent. They should support access to phone-based care, while working to expand digital access.
Lawmakers should also continue supporting research and the development of standards to improve healthcare quality measures. Quality measures help ensure that all care, including care provided in a virtual setting, is high-quality and equitable.
While they are working on those policies, lawmakers should work toward the broader goal of digital equity. This includes bolstering basic internet infrastructure and advancing policies to make internet access and internet-connected devices more affordable.
New policies should also help ensure everyone has the knowledge and support needed to navigate the online world. The ability to navigate is critical to enabling full access to and participation in an increasingly digital society where people need reliable high-speed internet to apply for jobs, access online education and financial resources, and more. This makes digital equity a key element of social health — the nonmedical factors that significantly influence health outcomes.
If we want better health outcomes for all, we need to work to create digital equity and make expanded telehealth policies permanent to give more Americans access to much needed care.
Learn more about digital equity and public policy by watching our December 2022 forum with leading experts.
-
Social Share
- Share Lawmakers Must Act to Boost Telehealth and Digital Equity on Pinterest
- Share Lawmakers Must Act to Boost Telehealth and Digital Equity on Linkedin
- Share Lawmakers Must Act to Boost Telehealth and Digital Equity on Twitter
- Share Lawmakers Must Act to Boost Telehealth and Digital Equity on Facebook
- Print Lawmakers Must Act to Boost Telehealth and Digital Equity
- Email Lawmakers Must Act to Boost Telehealth and Digital Equity

August 19, 2024
AI in health care: 7 principles of responsible use
These guidelines ensure we use artificial intelligence tools that are safe …

July 22, 2024
Our nation’s health depends on well-funded research
Advanced medical science improves patient outcomes. We urge lawmakers to …

July 16, 2024
Teacher residency program improves retention and diversity
A $1.5 million Kaiser Permanente grant addresses Colorado teacher shortage …

June 19, 2024
Investments in Black community promote total health for all
Funding from Kaiser Permanente in Washington helps to promote mental health, …

May 24, 2024
Investing to meet health care needs
The new Wildomar Trail Medical Offices offer additional opportunities for …

May 7, 2024
Making cancer care more convenient in Southern California
Kaiser Permanente has opened a new Radiation Oncology Center at the Bellflower …

May 7, 2024
Can the badly broken prescription drug market be fixed?
Prescription drugs are unaffordable for millions of people. With the right …

April 12, 2024
It’s time to address America’s Black maternal health crisis
Health care leaders and policymakers should each play their part to help …

April 9, 2024
Denver Fire Department annual blood work screenings triple
It’s easy to put off recommended health screenings, and sometimes even …

April 8, 2024
Reducing inequity with fruits and vegetables
Black Americans experience worse health outcomes compared to other populations …

March 26, 2024
Donations assure access to affordable health care
Kaiser Permanente grant and challenge spark $18.7 million for Denver Health’s …

March 19, 2024
Fostering responsible AI in health care
With the right policies and partnerships, artificial intelligence can lead …

March 18, 2024
Program helps member prioritize her health
Medical Financial Assistance program supports access to health care.

March 6, 2024
Former employee honored for supporting South LA families
Bill Coggins, who founded the Kaiser Permanente Watts Counseling and Learning …
March 4, 2024
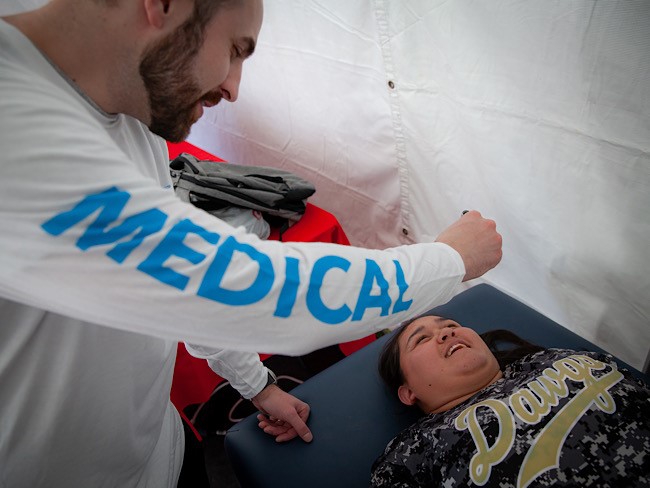
Taking care of Special Olympics athletes
Kaiser Permanente physicians and medical students provide medical exams …

February 26, 2024
Patients can apply for help with medical bills
Kaiser Permanente offers financial assistance for people struggling to …

February 12, 2024
Proposition 1 would bolster mental health care in California
Kaiser Permanente supports the ballot measure to expand and improve mental …

February 2, 2024
Expanding medical, social, and educational services in Watts
Kaiser Permanente opens medical offices and a new home for the Watts Counselin …

January 31, 2024
Prioritizing policies for health and well-being in Colorado
CityHealth’s 2023 Annual Policy Assessment awards cities for their policies …

January 22, 2024
Solutions for strengthening the mental health care workforce
Better public policies can help address the challenges. We encourage policymak …

January 10, 2024
‘You don’t know unless you ask them’
Kaiser Permanente’s Patient Advisory Councils help us create exceptional …

December 20, 2023
Funding solutions to end gun violence
Researchers and organizations are exploring inventive ways to reduce gun …

December 20, 2023
Championing inclusivity at the Fall Games
Kaiser Permanente celebrates inclusion at Special Olympics Southern California …

December 15, 2023
Climate change is already affecting our health
The health care industry is responsible for 8% to 10% of harmful emissions …

December 7, 2023
Safe, secure housing is a must for health
We offer housing-related legal help to prevent evictions and remove barriers …

December 6, 2023
Video prenatal visits are a boon for a busy working mom
A new care option offers a mix of in-person and virtual visits, supported …

December 6, 2023
Solid foundation: How construction careers support health
Steady employment can improve a person's health and well-being. Our new …

November 13, 2023
Congress must act to address drug shortages
Kaiser Permanente is working to address drug shortages and support policies …

November 9, 2023
Announcing the Common Health Coalition
Kaiser Permanente, AMA, AHA, ACHP, and AHIP join to strengthen the partnership …

November 1, 2023
Meet our 2023 to 2024 public health fellows
To help develop talented, diverse community leaders, Kaiser Permanente …

October 11, 2023
Expanded gun violence prevention efforts
The next phase for the Kaiser Permanente Center for Gun Violence Research …

September 29, 2023
2022 in review: A focus on equity, quality, and community
Our annual report shows how our dedicated employees and physicians provided …

September 19, 2023
Is telehealth right for you?
Members give video visits high marks — and with a few simple tips, you …

September 6, 2023
Advancing mental health crisis care through public policy
Organizations that provide public mental health crisis services must work …

August 28, 2023
Grants improve the total health of our communities
Kaiser Permanente increases access to mental health services in Southern …

August 16, 2023
Cervical cancer screening: Exploring the at-home HPV test
Kaiser Permanente is at the forefront of cervical cancer research. Find …

August 15, 2023
'Hot-spot' strategy gets more Californians vaccinated
A new location-based vaccine strategy by Kaiser Permanente was successful …

August 10, 2023
Highlighting our community health work in Southern California
The Kaiser Permanente Southern California 2022 Community Health Snapshot …

August 2, 2023
Social health resources are just a click or call away
The Kaiser Permanente Community Support Hub can help members find community …

July 11, 2023
Our prescription for safe, effective, more affordable drugs
Our approaches ensure effectiveness and safety, and drive cost savings. …

June 30, 2023
Our response to Supreme Court ruling on LGBTQIA+ protections
Kaiser Permanente addresses the Supreme Court decision on LGBTQIA+ protections …

June 29, 2023
Our response to Supreme Court's ruling on affirmative action
Kaiser Permanente addresses the Supreme Court decision on affirmative action …

June 29, 2023
Special Olympics athletes go for the gold
Kaiser Permanente celebrated its sixth year as official health partner …

June 14, 2023
Honored for commitment to people with disabilities
The Achievable Foundation recognized Kaiser Permanente for its work to …

June 7, 2023
Engaging businesses for action on climate and health equity
New climate collaborative with BSR announced at joint Kaiser Permanente …

June 1, 2023
Policy recommendations from a mental health therapist in training
Changing my career and becoming a therapist revealed ways our country can …

May 30, 2023
Kaiser Permanente commits up to $10 million to Denver Health
Funding comes as Denver Health provided $120 million in uncompensated care …

May 30, 2023
Volunteer-driven clinic offers free care in Washington
The annual Seattle King County Clinic brings health care to low-income …

May 22, 2023
Investing and partnering to build healthier communities
Kaiser Permanente supports Asian Americans Advancing Justice to promote …

May 19, 2023
Partnering to improve the health of homeless individuals
Grant funds will combat housing inaccessibility and improve health care …

May 11, 2023
COVID-19 testing, testing — Get results in 1, 2, 3
Testing is the most important way you can help control the spread of COVID-19.

May 10, 2023
A workplace for all
We value and respect employees and physicians of all backgrounds, identities, …

May 10, 2023
Equity, inclusion, and diversity
We strive for equity and inclusion for all.

May 2, 2023
Women lead an industrial revolution at the Kaiser Shipyards
Early women workers at the Kaiser shipyards diversified home front World …

April 27, 2023
Inspiring students to pursue health care careers
Kaiser Permanente is confronting future health care staffing challenges …

April 25, 2023
Hannah Peters, MD, provides essential care to ‘Rosies’
When thousands of women industrial workers, often called “Rosies,” joined …

April 11, 2023
Collaboration is key to keeping people insured
With the COVID-19 public health emergency ending, states, community organizati …

April 7, 2023
Virtual care helps ease physical pain
Kaiser Permanente offers many high-quality, convenient options to help …

April 7, 2023
Increasing access to health care
Kaiser Permanente launches new mobile health vehicle on Oahu.

April 5, 2023
Housing help brings stability to patients’ lives
With medical-legal partnerships, we’re helping prevent evictions.

April 3, 2023
Hospital patients who are homeless connected to housing
A Kaiser Permanente program connects patients experiencing homelessness …

March 29, 2023
Supporting a safer future with public health
We’re partnering on 3 initiatives to strengthen public health in the United …

March 28, 2023
Sentenced to prison, not a life of bad health
Reentering society after serving time can land people in unhealthy situations. …

March 14, 2023
Named among World’s Most Ethical Companies for 5th time
Organizations that receive this recognition improve communities, build …

March 13, 2023
Making waves with our first female sports ambassador
Kaiser Permanente in Southern California partners with San Diego Wave Fútbol …

March 7, 2023
Hiring alone won’t solve the health care worker shortage
For America to build — and keep — a health care workforce big enough to …

March 2, 2023
Improving the health of the community
Kaiser Permanente awards $80,000 in grants for health policy and community …

February 28, 2023
A conversation about pregnancy and women’s heart health
New research shows blood pressure patterns early in pregnancy can identify …

February 17, 2023
Good health starts in our communities: 2022 by the numbers
Kaiser Permanente supports total health in our communities in partnership …

February 3, 2023
Addressing health and housing insecurity
Kaiser Permanente supports 3 Hawaii-based nonprofits.

February 2, 2023
Addressing social isolation in the Northwest
Kaiser Permanente invests $3.3 million to build healthy social connections …

January 27, 2023
Timely flu vaccinations at community events
Proactive flu prevention outreach in Downey, California.

November 16, 2022
Passport to preventive care
Special event helps Latino community ensure their flu vaccinations and …

November 14, 2022
It’s time to rethink health care quality measurement
To meaningfully improve health equity, we must shift our focus to outcomes …
November 11, 2022
Early leaders in equity and inclusion
Explore Kaiser Permanente’s commitment to equitable, culturally responsive …
November 11, 2022
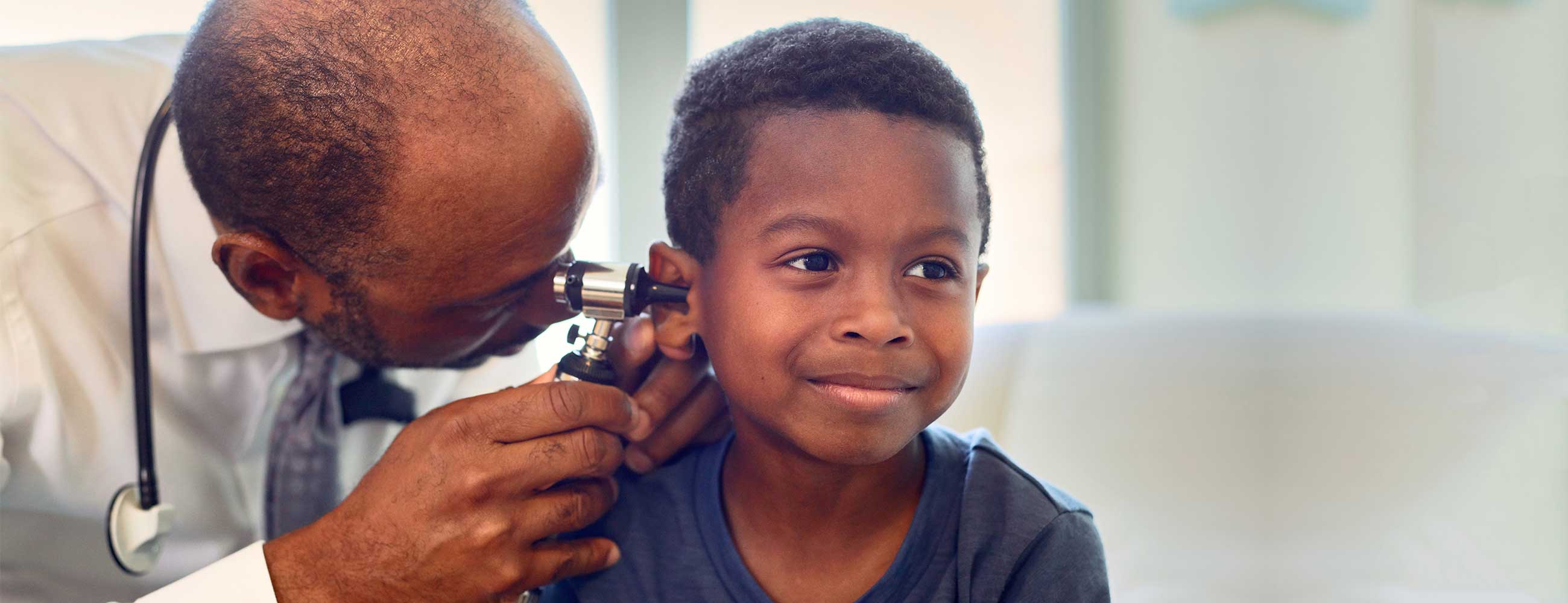
High-quality, equitable care
We believe everyone has a right to good health.

November 9, 2022
Applauding California’s ban on flavored tobacco
Voters passed Proposition 31, allowing the law banning these addictive …

November 8, 2022
Protecting access to medical care for legal immigrants
A statement of support from Kaiser Permanente chair and CEO Greg A. Adams …

October 26, 2022
Watts community project reaches construction milestone
Our expansion in Watts is part of a broader community health commitment …

September 29, 2022
Partnerships create pathways and launch dreams for youth
Collaboration offers ambitious young people an introduction to a health …

September 27, 2022
Maternity appointments from the comfort of home
New care option offers pregnant patients a mix of in-person and video visits.

September 16, 2022
Voter participation advances equity
National Voter Registration Day aims to register eligible voters and ensure …

September 14, 2022
Rent reporting can help millions build credit and thrive
A good credit score can make it easier to buy a home, pay for school, or …

September 13, 2022
Creating tobacco-free communities
Kaiser Permanente backs national efforts to ban flavored tobacco.

September 9, 2022
Minority youth mental health may not be elementary
Support, talk about, and advocate for kids’ mental health. Otherwise, greater …

August 17, 2022
2021 annual report sheds light on another challenging year
We reflect on 3 major COVID-19 surges, urgent vaccination efforts, and …

August 16, 2022
Our support for the Inflation Reduction Act
A statement from chair and chief executive Greg A. Adams on the importance …
August 12, 2022
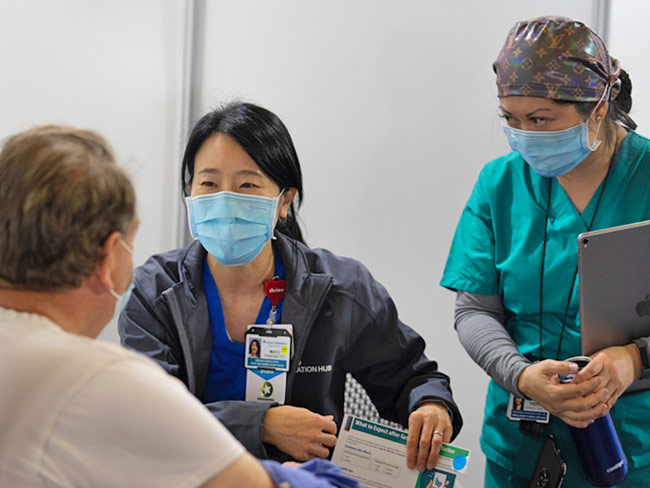
Preserving affordable health care coverage for millions
Congress should act to make COVID-19 policies permanent and ensure millions …

August 9, 2022
Getting care while traveling just got easier
Kaiser Permanente’s agreement with Cigna provides more convenient access …

August 8, 2022
Kaiser Permanente and Medical Teams launch mobile services
Mobile dental and medical clinics are now available for uninsured individuals …

June 23, 2022
Collaborative care for serious mental health conditions
An innovative telehealth program gives patients direct access to pharmacists …

June 16, 2022
Leadership and innovation to prevent gun injuries and deaths
Kaiser Permanente’s new Center for Gun Violence Research and Education …

May 29, 2022
Gun violence is a public health crisis. A preventable one.
We must do more to prevent gun violence and educate on its health implications …

May 27, 2022
Grants help AAPI communities and businesses
Kaiser Permanente is working with community organizations and businesses …

May 27, 2022
The importance of connecting patients with social resources
In Oregon and Southwest Washington, Kaiser Permanente is helping members …

May 18, 2022
Lifestyle coaching lowers blood pressure in Black adults
Kaiser Permanente study finds culturally tailored program leads to long-term …

May 4, 2022
Donated supplies keep community organizations pandemic-ready
We donated over $28 million worth of face masks, hand sanitizer, and other …

May 2, 2022
How to transform mental health care: Follow the research
We applaud President Biden and Congress as they begin to set policies that …

April 26, 2022
Employee-owned businesses foster healthier local economies
When employees share in the wealth of their company, the community benefits. …

April 19, 2022
Medical school ranks among nation’s most diverse
The ranking reflects the Kaiser Permanente Bernard J. Tyson School of Medicine …