'Hot-spot' strategy gets more Californians vaccinated
A new location-based vaccine strategy by Kaiser Permanente was successful in addressing COVID-19 vaccination disparities among underserved communities.
A targeted vaccination strategy helped Kaiser Permanente achieve an overall vaccination rate of 81% among all Southern California members.
In addition to bringing isolation and illness to the world, the COVID-19 pandemic spotlighted the health disparities among Southern California communities.
By January 2021, when the first COVID-19 vaccines became available to the public, it was clear that some communities with fewer resources were seeing higher rates of illness and death due to COVID-19. Getting vaccines and making them widely available was a challenge in Southern California and across the nation.
At Kaiser Permanente, teams from the Southern California Permanente Medical Group and the Southern California Department of Research & Evaluation partnered to address the issue. A study outlining these efforts was published on March 13, 2023, in The Permanente Journal and is featured in the Department of Research & Evaluation’s 2022 Annual Report.
Limited socioeconomic opportunities, such as a good education and a stable job, as well as biased policies and attitudes disproportionately affect underrepresented populations and their health outcomes. These factors contributed significantly to the unequal access to vaccines that occurred throughout the United States in 2021, according to Reina Haque, PhD, an epidemiologist with the Department of Research & Evaluation, who was the senior author on the study.
‘Hot-spot’ strategy employed to address inequities
“To address the challenges of inequitable access to the COVID-19 vaccine in Southern California, Kaiser Permanente applied a community-oriented and geographic strategy aimed at reducing disparities in COVID-19 vaccination by ZIP codes,” said Haque.
This became known as the “hot-spot” strategy.
Researchers used analytical tools to assess the risk of COVID-19 in different communities within Kaiser Permanente’s 670 Southern California ZIP codes. This produced monthly lists of ZIP codes that required additional health care resources and vaccination strategies. Then the COVID-19 vaccination teams worked with Kaiser Permanente medical centers to get more people vaccinated in the identified ZIP codes.
They sent proactive texts, extended vaccination clinic hours, provided in-home vaccinations for home-bound patients, and had a mobile health vehicle with vaccines drive into neighborhoods. Health care providers at various pop-up clinics and in the mobile health vehicle vaccinated both Kaiser Permanente members and nonmembers.
“The strategy was effective in both creating awareness of inequities and guiding vaccination efforts toward the most vulnerable communities,” said Haque.
Strategy success leads to further efforts
By the end of 2021, this hot-spot strategy helped Kaiser Permanente achieve an overall vaccination rate of 81% among all Southern California members. Additionally, 2 out of 3 people who received a vaccination through the hot spot-guided mobile health vehicle were Hispanic or Black.
But the work didn’t stop there. This place-based approach to reducing vaccination disparities in underserved communities was quickly adapted to other health disparities.
In 2022, the strategy was used to address disparities in flu vaccination and diabetes control.
“After we had successfully employed this hot-spot vaccination strategy with COVID-19, we were able to refine how we analyzed the data and our approach to the social and economic factors impacting our members,” said Alexander Martos, DrPH, interim director for the Southern California Permanente Medical Group’s Equity, Inclusion, and Diversity department. “We are now in the process of operationalizing these hot spots with our vaccination and proactive care teams and look forward to exploring new health equity opportunities in the future.”
Read more inspiring stories that exemplify the spectrum of our research’s impact in the Southern California Department of Research & Evaluation 2022 Annual Report.
-
Social Share
- Share ‘Hot-Spot’ Strategy Gets More Californians Vaccinated on Pinterest
- Share ‘Hot-Spot’ Strategy Gets More Californians Vaccinated on LinkedIn
- Share ‘Hot-Spot’ Strategy Gets More Californians Vaccinated on Twitter
- Share ‘Hot-Spot’ Strategy Gets More Californians Vaccinated on Facebook
- Print ‘Hot-Spot’ Strategy Gets More Californians Vaccinated
- Email ‘Hot-Spot’ Strategy Gets More Californians Vaccinated

January 16, 2026
The importance of childhood vaccinations
Kaiser Permanente continues to recommend the vaccines that have been on …

December 12, 2025
Quick on-site blood sugar tests target uncontrolled diabetes
A new research study by Kaiser Permanente shows point-of-care A1C testing …

December 5, 2025
The importance of hepatitis B vaccination for newborns
Kaiser Permanente will continue to offer the hepatitis B vaccine at birth …

November 4, 2025
A best place to work for veterans
As a 2025 top Military Friendly Employer, Kaiser Permanente supports veterans …

October 15, 2025
Kaiser Permanente shows up strong for the annual plane pull
Championing health equity and teamwork drives Kaiser Permanente’s support …

June 26, 2025
Our commitment to vaccine access
Kaiser Permanente’s statement on vaccine access.

March 27, 2025
We’re committed to mentorship, mental health, and communities
Kaiser Permanente awarded Elevate Your G.A.M.E. a grant to expand program …

March 25, 2025
AI in health care: 7 principles of responsible use
These guidelines ensure we use artificial intelligence tools that are safe …

March 17, 2025
Remembering Bill Coggins and his lasting legacy
The founder of the Kaiser Permanente Watts Counseling and Learning Center …

December 26, 2024
Linking isolated communities to care
A collaborative partnership, powered by trusted nonprofit partners, brings …

November 11, 2024
Health care coverage now accessible to uninsured people
Indigenous farmworkers may qualify for new Kaiser Permanente coverage.

November 11, 2024
Medicare telehealth flexibilities should be here to stay
We urge Congress to extend policies that have improved access to care and …

October 15, 2024
Our dedication to fostering well-being and equity
The 2023 Kaiser Permanente Southern California Community Health County …

September 16, 2024
Voting affects the health of our communities
In honor of National Voter Registration Day, we encourage everyone who …

July 16, 2024
Teacher residency program improves retention and diversity
A $1.5 million Kaiser Permanente grant addresses Colorado teacher shortage …

June 19, 2024
Investments in Black community promote total health for all
Funding from Kaiser Permanente in Washington helps to promote mental health, …

May 7, 2024
Can the badly broken prescription drug market be fixed?
Prescription drugs are unaffordable for millions of people. With the right …

April 12, 2024
It’s time to address America’s Black maternal health crisis
Health care leaders and policymakers should each play their part to help …

March 18, 2024
Program helps member prioritize her health
Medical Financial Assistance program supports access to health care.

March 6, 2024
Former employee honored for supporting South LA families
Bill Coggins, who founded the Kaiser Permanente Watts Counseling and Learning …
March 4, 2024
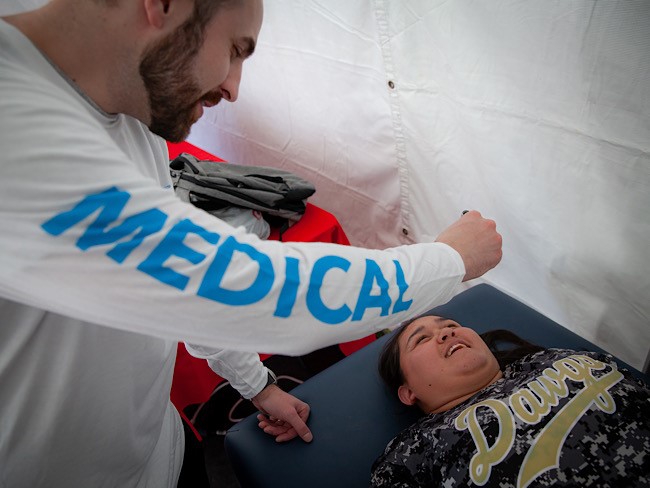
Taking care of Special Olympics athletes
Kaiser Permanente physicians and medical students provide medical exams …

February 2, 2024
Expanding medical, social, and educational services in Watts
Kaiser Permanente opens medical offices and a new home for the Watts Counseling …

December 20, 2023
Championing inclusivity at the Fall Games
Kaiser Permanente celebrates inclusion at Special Olympics Southern California …

December 7, 2023
Safe, secure housing is a must for health
We offer housing-related legal help to prevent evictions and remove barriers …

December 6, 2023
Solid foundation: How construction careers support health
Steady employment can improve a person's health and well-being. Our new …

November 1, 2023
Meet our 2023 to 2024 public health fellows
To help develop talented, diverse community leaders, Kaiser Permanente …
October 10, 2023
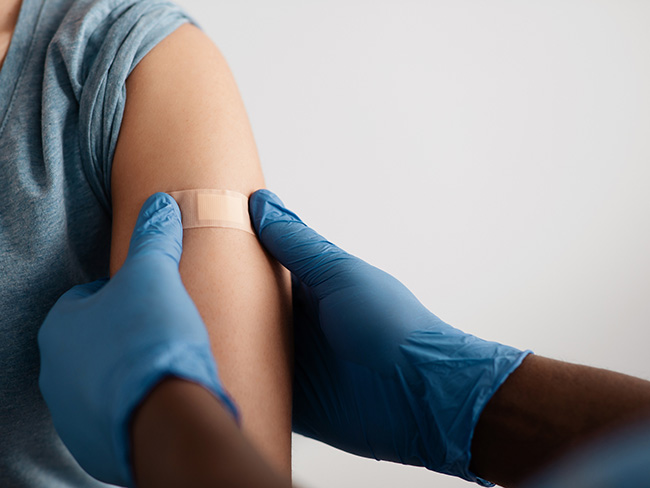
What to know about COVID-19 vaccines
The updated vaccine is recommended for everyone 6 months and older.

August 17, 2023
Beyond clinic walls: Research supporting healthy communities
Stories in the Department of Research & Evaluation 2022 Annual Report demonstrate …

August 10, 2023
Highlighting our community health work in Southern California
The Kaiser Permanente Southern California 2022 Community Health Snapshot …

August 2, 2023
Social health resources are just a click or call away
The Kaiser Permanente Community Support Hub can help members find community …

June 30, 2023
Our response to Supreme Court ruling on LGBTQIA+ protections
Kaiser Permanente addresses the Supreme Court decision on LGBTQIA+ protections …

June 29, 2023
Our response to Supreme Court's ruling on affirmative action
Kaiser Permanente addresses the Supreme Court decision on affirmative action …

June 29, 2023
Special Olympics athletes go for the gold
Kaiser Permanente celebrated its sixth year as official health partner …

June 14, 2023
Honored for commitment to people with disabilities
The Achievable Foundation recognized Kaiser Permanente for its work to …

June 7, 2023
Engaging businesses for action on climate and health equity
New climate collaborative with BSR announced at joint Kaiser Permanente …

May 22, 2023
Investing and partnering to build healthier communities
Kaiser Permanente supports Asian Americans Advancing Justice to promote …

May 16, 2023
COVID-19 public health emergency has ended: What’s changed?
Vaccinations, testing, and treatment are still widely accessible. Member …

May 11, 2023
COVID-19 testing, testing — Get results in 1, 2, 3
Testing is the most important way you can help control the spread of COVID-19.

May 10, 2023
A workplace for all
We are building inclusive work and care environments where everyone feels …

May 10, 2023
Health equity, inclusion, and belonging
We strive for fairness, respect, and inclusion for all.

May 2, 2023
Women lead an industrial revolution at the Kaiser Shipyards
Early women workers at the Kaiser shipyards diversified home front World …

April 27, 2023
Inspiring students to pursue health care careers
Kaiser Permanente is confronting future health care staffing challenges …

April 25, 2023
Hannah Peters, MD, provides essential care to ‘Rosies’
When thousands of women industrial workers, often called “Rosies,” joined …

April 11, 2023
Collaboration is key to keeping people insured
With the COVID-19 public health emergency ending, states, community organizations, …

April 5, 2023
Housing help brings stability to patients’ lives
With medical-legal partnerships, we’re helping prevent evictions. Patients …

April 3, 2023
Hospital patients who are homeless connected to housing
A Kaiser Permanente program connects patients experiencing homelessness …

March 29, 2023
Supporting a safer future with public health
We’re partnering on 3 initiatives to strengthen public health in the United …

February 17, 2023
Good health starts in our communities: 2022 by the numbers
Kaiser Permanente supports total health in our communities in partnership …

January 17, 2023
Lawmakers must act to boost telehealth and digital equity
Making key pandemic-era telehealth policies permanent and ensuring more …

November 14, 2022
It’s time to rethink health care quality measurement
To meaningfully improve health equity, we must shift our focus to outcomes …
November 11, 2022
High-quality, equitable care
We believe everyone has a right to good health.
November 11, 2022
Early leaders in equity and inclusion
Explore Kaiser Permanente’s commitment to equitable, culturally responsive …

November 8, 2022
Protecting access to medical care for legal immigrants
A statement of support from Kaiser Permanente chair and CEO Greg A. Adams …

March 22, 2022
Our commitment to equity and our LGBTQIA+ communities
A statement from chair and chief executive officer Greg A. Adams.

February 21, 2022
A best place to work for LGBTQ+ equality
Human Rights Campaign Foundation gives Kaiser Permanente another perfect …
February 14, 2022
Health care scholarships available
Kaiser Permanente in Hawaii to provide up to $100,000 in scholarships to …

November 30, 2021
Bechara Choucair, MD, returns as chief health officer
After serving on the White House COVID-19 response team, Bechara Choucair, …

October 12, 2021
Beyond advocacy: Requiring vaccination to stop COVID-19
Kaiser Permanente and other leading companies are mandating COVID-19 shots …

August 25, 2021
Kaiser Permanente’s history of nondiscrimination
Our principles of diversity and our inclusive care began during World War …

July 7, 2021
Achieving health equity
Equal medical care is not enough to end disparities in health outcomes.

June 2, 2021
Path to employment: Black workers in Kaiser shipyards
Kaiser Permanente, Henry J. Kaiser’s sole remaining institutional legacy, …
March 11, 2021
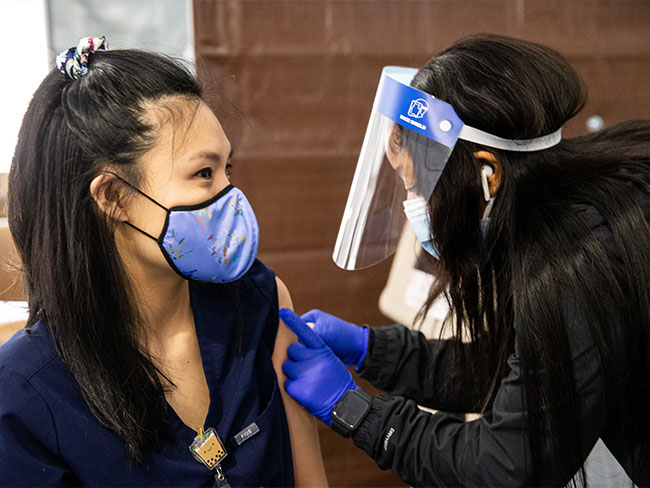
Our support of the American Rescue Plan Act
A statement from CEO Greg A. Adams about the American Rescue Plan Act.

May 18, 2020
Nurses step up in crises
Kaiser Permanente nurses have been saving lives on the front lines since …

November 8, 2019
Swords into stethoscopes — veterans in health professions
Kaiser Permanente has actively hired veterans in all capacities since World …

August 28, 2019
When labor and management work side by side
From war-era labor-management committees to today’s unit-based teams, cooperation …

June 5, 2019
Breaking LGBT barriers for Kaiser Permanente employees
“We managed to ultimately break through that barrier.” — Kaiser Permanente …

March 29, 2019
Equal pay for equal work
Kaiser shipyards in Oregon hired the first 2 female welders at equal pay …

March 8, 2018
Slacks, not slackers — women’s role in winning World War II
Women who worked in the Kaiser shipyards helped lay the groundwork for …

February 22, 2018
The amazing true story of Park Ranger Betty Reid Soskin
She is the oldest national park ranger in the country with a legacy of …

October 12, 2017
An experiment named Fabiola
Health care takes root in Oakland, California.

August 10, 2017
‘Good medicine brought within reach of all'
Paul de Kruif, microbiologist and writer, provides early accounts of Kaiser …

March 7, 2017
Beatrice Lei, MD: From Shantou, China, to Richmond, California
She served as a role model and inspiration to the women physicians and …
March 1, 2017
Screening for better health: Medical care as a right
When industrial workers joined the health plan, an integrated battery of …

February 3, 2017
Ellamae Simmons — trailblazing African American physician
Ellamae Simmons, MD, worked at Kaiser Permanente for 25 years, and to this …

May 5, 2016
Male nursing pioneers
Groundbreaking male students diversify the Kaiser Foundation School of …
April 27, 2015
Eugene Hickman, MD — Pioneering Black physician
Dr. Hickman had a long career at Kaiser Permanente, becoming president …

May 5, 2014
Black nurses get together to forge their own future
California African American nurses organize in early 1970s to address health …

May 1, 2014
Beloved nurse earned place in Kaiser Permanente history
Jessie Cunningham, the first Black nursing supervisor at Oakland Medical …

February 18, 2014
Alva Wheatley: Champion of Kaiser Permanente diversity
Third in a series marking Black History Month.

January 31, 2014
Raleigh Bledsoe, MD: First Black radiologist west of Rockies
Dr. Bledsoe became the first Black physician for Southern California Permanente …

August 2, 2013
Image of Rosie broadens to embrace African American women
Black women find new opportunities to elevate work status on the World …

July 15, 2013
Labor unions offer early support for nascent Permanente Health Plan
After World War II, the experience of the Kaiser Permanente Health Plan …

December 1, 2011
Kaiser Permanente’s early struggle to stand up to AIDS
New challenges provided collaborative opportunities for Kaiser Permanente …

April 30, 2011
Nurses begin quest for professional recognition after World War II
Co-founder Dr. Sidney Garfield makes history by signing the first nurse …