Can the badly broken prescription drug market be fixed?
Prescription drugs are unaffordable for millions of people. With the right policy solutions, we can get back on the path to affordability.
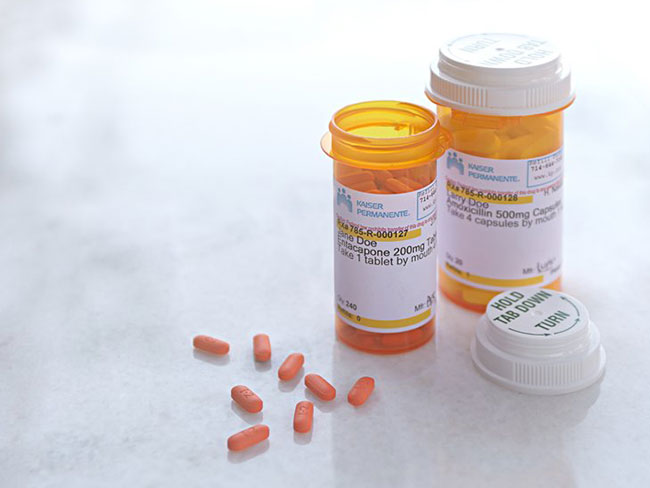
The high cost of prescription drugs is making them unaffordable for patients.
In a free market, sellers compete on price, and buyers choose the lowest priced good that meets their needs. It’s a fundamental law of economics.
But in the real world, this law sometimes crumbles — especially in America’s prescription drug market.
Drugmakers rarely compete on price. This is one reason why the U.S. spent over $633 billion on prescription drugs last year.
Compared with other high-income countries, the U.S. has the highest per capita prescription drug spending.
How government policies led to higher drug prices
Starting in 1990, a series of policy changes undermined any leverage buyers had to help rein in rising costs.
- Medicaid Drug Rebate Program — Congress introduced the Medicaid Drug Rebate Program in 1990. Under this law, in exchange for having all of their drugs covered, drugmakers agree to pay rebates to state Medicaid programs. Because the law requires that Medicaid receive the “best price,” manufacturers cannot offer deeper discounts to private purchasers. This price floor means Americans with private health insurance (that is, most Americans) pay higher prices for drugs and higher premiums for drug coverage than they otherwise could.
- Health plans covering most drug costs — Over time, health plans have paid for a larger share of the total cost of prescription drugs. Even before Medicare started offering prescription drug coverage in 2006, consumers had become more insulated from the full price of drugs. This helped consumers afford their medications. But patients and their doctors are often unaware of the full price of a drug. They have no reason to seek or choose an equally effective, lower-priced alternative.
- Loopholes in patent laws — When the federal government grants a drugmaker a patent, only the company that holds the patent can make and sell the drug for a period of time. Without competition, these drugmakers can set whatever price they like. Patents are important to stimulate innovation. But there are loopholes. In some cases, drugmakers get patents — and great financial rewards — based on publicly financed drug research. Sometimes they build a complex web of patents. Called patent thickets, these webs make it much harder for competitors to come to market.
This combination of policies has allowed manufacturers to raise prices relentlessly without fear of political or market consequences.
Policy solutions
The broken prescription drug market makes health care unaffordable for millions. But we have some policy options, including:
- Addressing anticompetitive behavior. We can build a fairer patent system. New legislation in Congress addresses patent thickets and more.
- Increasing the use of biosimilars. At Kaiser Permanente, we use the biosimilar versions of drugs whenever possible. They’re equally effective and less expensive. For example, we’ve switched most of our members to the newest biosimilar for Humira, a prescription medication for rheumatoid arthritis and other inflammatory diseases. This saved close to $300 million in 2023 alone.
Humira has a list price of $7,000. By switching members to the biosimilar, we lowered costs for our members and employer groups. Congress should make it easier for doctors to use biosimilars with their patients.
- Focusing on the evidence of a drug’s safety and efficacy. We pay far too much for drugs that don’t improve health outcomes or that show little value over alternative treatments. New policies should strengthen how the Food and Drug Administration approves drugs. This will ensure that available drugs are safe and work well.
- Strengthening Medicare’s ability to negotiate drug prices. Thanks to a law passed in 2022, Medicare can now negotiate the price of a few of the costliest drugs in the US. The drug industry is pushing back aggressively through lawsuits and heavy lobbying. Congress should stand firm and build on this law to protect both Medicare and its beneficiaries into the future.
- Tackling drug shortages. Shortages of specific drugs prevent patients from getting the treatment they need. These shortages also cause rising prices. It’s time our government did more to incentivize companies to make more generic (lower cost) drugs in America. And we need policies that compel drug manufacturers to share more information about their supply pipeline. Then health care systems and providers can identify problems earlier.
The prescription drug market is broken.
It’s time for our lawmakers to have some serious conversations about solutions. Patients deserve access to effective drugs at prices we all can afford.