When things fell apart, telehealth was her lifeline
Stuck at home during the pandemic, a Kaiser Permanente member with autoimmune disease relied on her phone and computer to connect to mental health support.
At age 63, Elizabeth was content. She was in a long-term relationship, enjoyed spending time with her adult daughters, and loved her job teaching deaf students at a Northern California middle school.
And 15 years after being hospitalized for severe depression, the Kaiser Permanente member had learned to cope with the sadness and anxiety she still experienced by working with a therapist and attending classes on topics such as couples’ communication and healthy living.
Then things began to unravel for Elizabeth (who asked that we use her first name only to protect her privacy). An autoimmune disease forced her to take early retirement and move to a more affordable home, and she and her partner broke up.
“I spiraled down into a very deep depression,” she said.
Connecting to intensive support
Elizabeth’s therapist, Sabrina Chaumette, a licensed clinical social worker, referred her to the Intensive Outpatient Program at the Kaiser Permanente Oakland Medical Center.
“It’s a program for people who are in crisis and need a high level of services, but they don’t need or want to be in the hospital,” Chaumette explained. “They come in 3 mornings a week and work with a psychiatrist who evaluates their medications and a team of providers who offer everything from mindfulness and cognitive behavioral therapy to life skills and help with issues such as job loss and housing problems.”
Slowly but surely, things began to improve for Elizabeth. Then the COVID-19 pandemic hit. At risk of severe illness due to her autoimmune disorder, she isolated herself at home, and her mental health took a turn for the worse.
“I was having a hard time even getting out of bed,” she said.
Bridging the digital divide
As Kaiser Permanente quickly transitioned most in-person appointments to phone and video to prevent the spread of the virus, Elizabeth struggled to adjust.
“I am technologically a dinosaur, and I needed a lot of help from the administrative staff to learn how to use the video platform,” she said. “And it was awkward and uncomfortable to be sitting in front of my laptop crying. I didn’t turn my video camera on for the first 3 months. But then I realized, this is my key to staying sane and getting healthy.”
In addition to her sessions with Chaumette, Elizabeth began participating in several telehealth groups for people living with depression, anxiety, and trauma.
“It’s been a real lifesaver for me throughout this difficult time,” she said. “I feel comfortable and seen.”
A virtual lifeline
On the days when she doesn’t have individual or group therapy, Elizabeth takes advantage of virtual health education classes through Kaiser Permanente East Bay Behavioral Health on topics such as improving sleep and reducing stress through mindfulness.
She’s also an avid user of the Calm self-care app, available to Kaiser Permanente members at no cost.
“I do the Daily Calm meditation every morning, and I fall asleep to a sleep story every night,” she said. “It’s gotten to the point where, when I open the app, my dogs know to come into the bedroom and lie down with me.”
Another turn in the road
Just as she began to feel comfortable going out into the world again, Elizabeth slipped while walking her 2 dogs, fracturing her ankle and injuring her foot.
“Not being able to walk or drive has forced me to rely on telehealth more than ever,” she said by email. “And it’s working. Prepping for the surgery and after-care have involved my phone, my computer, video visits, and a few miracles thrown in for good measure. I’ve kept going to all my mental health groups and appointments with no problems. What a story!”
Learn more about mental health care at Kaiser Permanente, and find out about ways to access care through telehealth.
-
Social Share
- Share When Things Fell Apart, Telehealth Was Her Lifeline on Pinterest
- Share When Things Fell Apart, Telehealth Was Her Lifeline on LinkedIn
- Share When Things Fell Apart, Telehealth Was Her Lifeline on Twitter
- Share When Things Fell Apart, Telehealth Was Her Lifeline on Facebook
- Print When Things Fell Apart, Telehealth Was Her Lifeline
- Email When Things Fell Apart, Telehealth Was Her Lifeline

May 7, 2025
How to cope with anxiety after childbirth
As a new mother, Cherissa Ong was overwhelmed by stress. A mental health …

March 29, 2025
We are meeting mental health care access requirements
The investments we’ve made over the last several years have resulted in …

February 25, 2025
Providing care to trauma survivors
Kaiser Permanente has been at the forefront of recognizing how trauma impacts …

December 26, 2024
How telehealth can make life easier for people with cancer
Virtual care connects cancer patients like Rob Tufel to a wide range of …

December 13, 2024
How to stay happy and healthy over the holidays
Sammie LaMont Moss, MD, a psychiatrist for Kaiser Permanente in Colorado, …

December 10, 2024
Accelerating growth in the mental health care workforce
Actions policymakers can take to grow and diversify the mental health care …

October 15, 2024
Our dedication to fostering well-being and equity
The 2023 Kaiser Permanente Southern California Community Health County …

October 10, 2024
Child anxiety relief: Therapy gets a digital boost
Shiloh Sevin’s well-being improves thanks to her psychologist and the Calm …
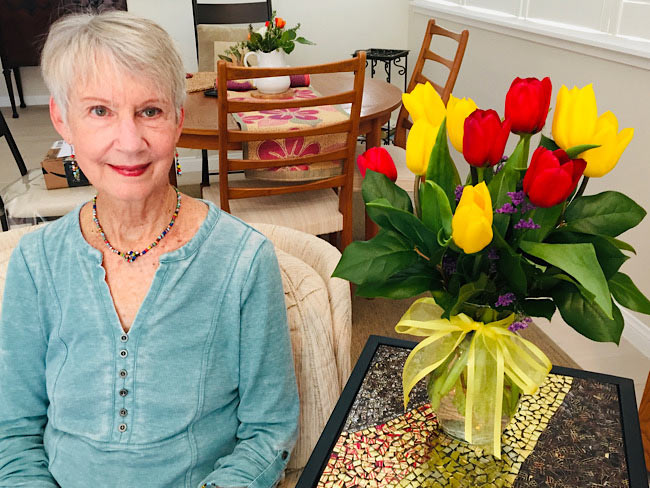
October 4, 2024
Teacher learns about herself and how to live with anxiety
A lifelong educator seeks behavioral health care to manage repetitive worries, …

October 1, 2024
From depression to connection: Older adult finds her way
After a long period of loneliness and isolation, Roberta Maguire gets the …

September 27, 2024
Youth suicide in the digital age is raising concerns
Young people face growing pressures from social media, school, and other …

September 27, 2024
Traumatized children find mental health therapy beneficial
A Ventura County community-based nonprofit provides counselors to help …

September 23, 2024
Meet KP Plus — Washington’s new large-group health plan of choice
This innovative plan more affordably adds choice and flexibility to Kaiser …

September 17, 2024
A Latina’s voice in mental health is impactful with her clients
Connecting through a shared heritage gives one therapist a unique perspective …

September 17, 2024
Groundbreaking at new medical offices in Pueblo
The new Pueblo North Medical Offices will replace the existing facility …

August 16, 2024
After severe depression, a ‘rainbow lit up my sky’
Shannon Parkin survived 7 suicide attempts. She shares her story of hope …

July 11, 2024
Transforming education and mental health in Watts
Our investment in the Watts neighborhood of California, in partnership …

June 27, 2024
5 facts about autism
A Kaiser Permanente doctor shares key details. By learning more about autism, …

May 24, 2024
Investing to meet health care needs
The new Wildomar Trail Medical Offices offer additional opportunities for …

May 14, 2024
A key ally in navigating mental health care for kids
Behavioral health consultants can provide a better understanding of often …

May 10, 2024
Self-care is key for new parents
Feeling emotional or overwhelmed after a new baby’s arrival? You’re not …

May 7, 2024
Making cancer care more convenient in Southern California
Kaiser Permanente has opened a new Radiation Oncology Center at the Bellflower …

May 3, 2024
Lonely and depressed — but not alone
After a lifetime of feeling isolated, Moth Wygal finds connection thanks …

April 10, 2024
For a new mom, talking about her worries helped her heal
One in 5 people experience depression, anxiety, or other mental health …

April 9, 2024
Denver Fire Department annual blood work screenings triple
It’s easy to put off recommended health screenings, and sometimes even …

March 26, 2024
Donations assure access to affordable health care
Kaiser Permanente grant and challenge spark $18.7 million for Denver Health’s …

March 18, 2024
Program helps member prioritize her health
Medical Financial Assistance program supports access to health care.

February 26, 2024
Patients can apply for help with medical bills
Kaiser Permanente offers financial assistance for people struggling to …

February 12, 2024
Proposition 1 would bolster mental health care in California
Kaiser Permanente supports the ballot measure to expand and improve mental …

February 2, 2024
Expanding medical, social, and educational services in Watts
Kaiser Permanente opens medical offices and a new home for the Watts Counseling …

January 29, 2024
Empowering minds to help others thrive
Supporting behavioral and mental health in communities where needs are …

January 22, 2024
Solutions for strengthening the mental health care workforce
Better public policies can help address the challenges. We encourage policymaker …

January 3, 2024
Addressing the shortage of mental health workers
There aren’t enough mental health professionals in the U.S. to meet the …

December 7, 2023
Safe, secure housing is a must for health
We offer housing-related legal help to prevent evictions and remove barriers …

December 6, 2023
Video prenatal visits are a boon for a busy working mom
A new care option offers a mix of in-person and virtual visits, supported …

November 29, 2023
Tapping into an array of mental health options
Pavan Somusetty, MD, explains how people who need support and guidance …

November 9, 2023
Announcing the Common Health Coalition
Kaiser Permanente, AMA, AHA, ACHP, and AHIP join to strengthen the partnership …

October 24, 2023
Childhood anxiety: What parents need to know
A child and adolescent psychiatrist shares tips on supporting your child …

October 11, 2023
Bridging the mental health gap
Kaiser Permanente’s partnership with Fontana Unified School District brings …

September 27, 2023
Harvest your power
Use biofeedback to help manage stress.

September 27, 2023
From suicide survivor to mental health advocate
Former Major League Baseball player Drew Robinson shares his story of hope …

September 19, 2023
Is telehealth right for you?
Members give video visits high marks — and with a few simple tips, you …

September 13, 2023
Mental health champion: A mission inspired by personal loss
San Diego Wave Fútbol Club star defender Naomi Girma, Kaiser Permanente …

September 6, 2023
Recovery from addiction is possible
Our clinicians help patients get the care they need to move forward with …

September 6, 2023
Advancing mental health crisis care through public policy
Organizations that provide public mental health crisis services must work …

August 28, 2023
Grants improve the total health of our communities
Kaiser Permanente increases access to mental health services in Southern …

August 16, 2023
Cervical cancer screening: Exploring the at-home HPV test
Kaiser Permanente is at the forefront of cervical cancer research. Find …

August 10, 2023
Successfully navigating the school year
These tips from Don Mordecai, MD, Kaiser Permanente’s national mental health …

August 4, 2023
Eating well and adopting healthy habits helps prevent cancer
Learn how lifestyle medicine is part of cancer care at Kaiser Permanente.

August 2, 2023
Social health resources are just a click or call away
The Kaiser Permanente Community Support Hub can help members find community …

June 30, 2023
Men's mental well-being is a priority
Unique challenges and societal pressures can impact men’s emotional well-being.

June 30, 2023
Our response to Supreme Court ruling on LGBTQIA+ protections
Kaiser Permanente addresses the Supreme Court decision on LGBTQIA+ protections …

June 28, 2023
Making waves to empower young girls
Kaiser Permanente and the San Diego Wave Fútbol Club host a second Wave …

June 23, 2023
Get the mental health support you need
Kaiser Permanente is here to help with care and valuable tools to support …

June 21, 2023
And that’s why they call postpartum the blues
Take time to adjust to a new baby and lifestyle changes — and reach out …

June 9, 2023
Mental health, addiction, and the power of a peer
Shared experience helps young people in Oregon build confidence for their …

June 7, 2023
Teen social media use may lead to depression
Creating a healthy relationship with social media can help safeguard the …

June 5, 2023
Understanding and living with bipolar disorder
A Kaiser Permanente member shares his personal journey of navigating bipolar …

June 1, 2023
Policy recommendations from a mental health therapist in training
Changing my career and becoming a therapist revealed ways our country can …

May 30, 2023
Kaiser Permanente commits up to $10 million to Denver Health
Funding comes as Denver Health provided $120 million in uncompensated care …

May 22, 2023
Sidelined by injury, a former nurse seeks depression care
Susan Sandhu struggled to find meaning in her life after an injury forced …

May 22, 2023
Investing and partnering to build healthier communities
Kaiser Permanente supports Asian Americans Advancing Justice to promote …

May 19, 2023
Partnering to improve the health of homeless individuals
Grant funds will combat housing inaccessibility and improve health care …

May 18, 2023
Addressing mental health trauma in a local community
Trauma-informed outreach efforts in Orange County are being recognized …

May 16, 2023
Managing trauma does not need to be traumatic
Expanded access to high-quality, affordable mental health care supports …

May 11, 2023
COVID-19 testing, testing — Get results in 1, 2, 3
Testing is the most important way you can help control the spread of COVID-19.

May 9, 2023
School shootings provoke anxiety in many children
Child psychiatrist defines anxiety, its symptoms, how to address it, and …

April 7, 2023
Virtual care helps ease physical pain
Kaiser Permanente offers many high-quality, convenient options to help …

April 7, 2023
Increasing access to health care
Kaiser Permanente launches new mobile health vehicle on Oahu.
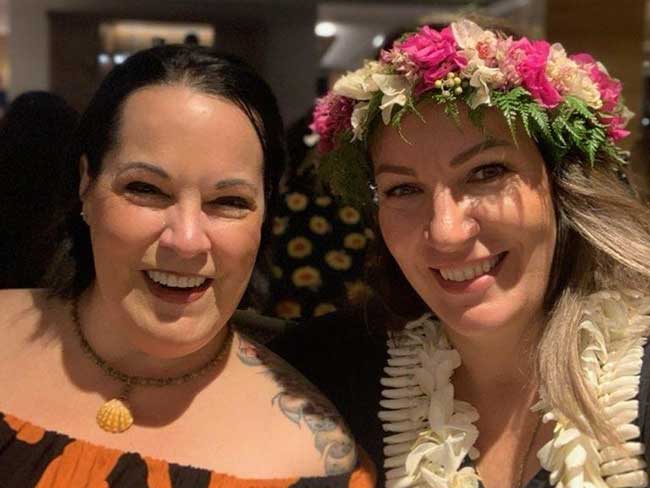
March 24, 2023
Finding hope after a mental health and addiction crisis
Treatment for bipolar disorder and opiate addiction helps a Kaiser Permanente …

March 13, 2023
Making waves with our first female sports ambassador
Kaiser Permanente in Southern California partners with San Diego Wave Fútbol …

March 7, 2023
For moments when you may not need to see a therapist
Kaiser Permanente provides members with convenient ways to improve their …

February 2, 2023
Addressing social isolation in the Northwest
Kaiser Permanente invests $3.3 million to build healthy social connections …

January 27, 2023
Timely flu vaccinations at community events
Proactive flu prevention outreach helped community members in Downey, California …

January 19, 2023
Understanding stress and how to manage it
A Kaiser Permanente psychiatrist shares advice for coping when stress won't …

January 17, 2023
Lawmakers must act to boost telehealth and digital equity
Making key pandemic-era telehealth policies permanent and ensuring more …
November 11, 2022
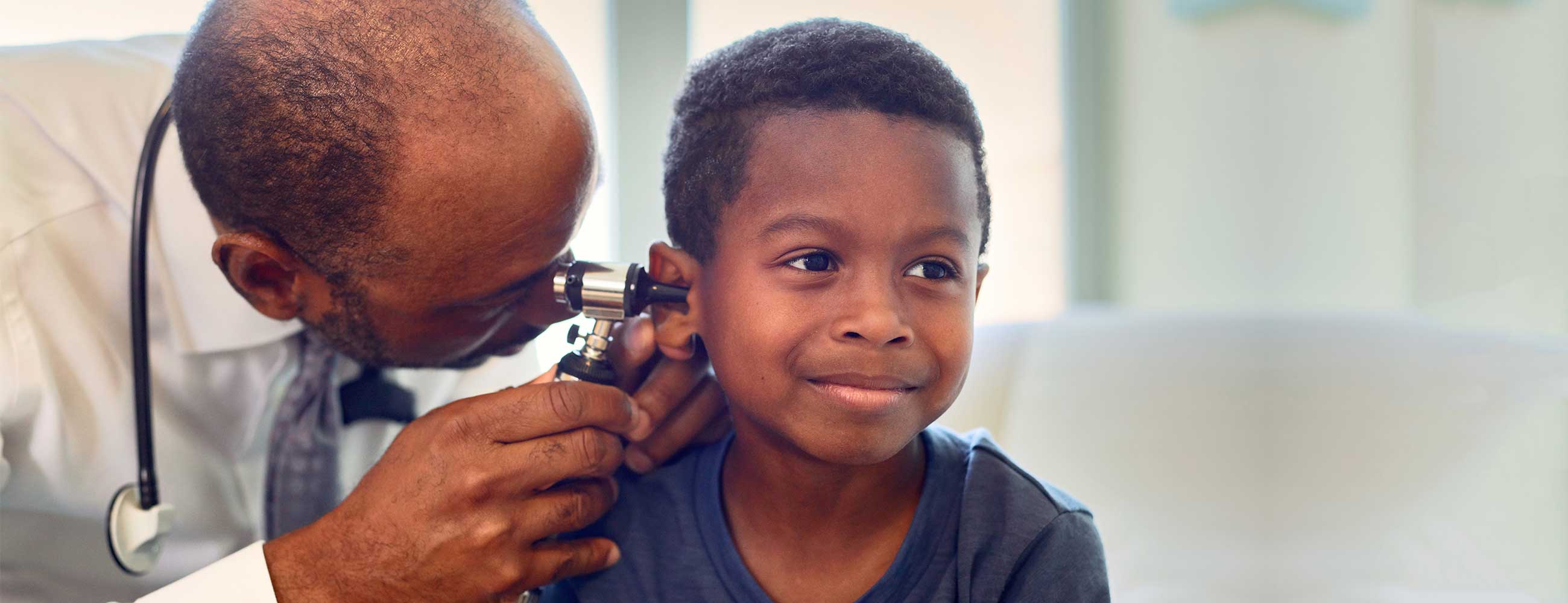
High-quality, equitable care
We believe everyone has a right to good health.

November 8, 2022
Protecting access to medical care for legal immigrants
A statement of support from Kaiser Permanente chair and CEO Greg A. Adams …

September 27, 2022
Maternity appointments from the comfort of home
New care option offers pregnant patients a mix of in-person and video visits.

September 7, 2022
How you can help prevent suicide
When someone you care about is struggling, it can be hard to know what …

August 29, 2022
For student athletes, mental wellness is a game changer
A sports medicine physician and mental health therapist discuss the mind-body …
August 12, 2022
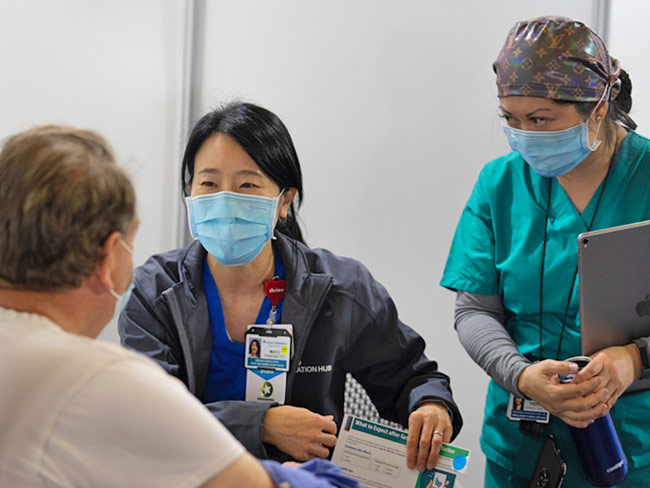
Preserving affordable health care coverage for millions
Congress should act to make COVID-19 policies permanent and ensure millions …

August 9, 2022
Getting care while traveling just got easier
Kaiser Permanente’s agreement with Cigna provides more convenient access …

August 8, 2022
Kaiser Permanente and Medical Teams launch mobile services
Mobile dental and medical clinics are now available for uninsured individuals …

August 3, 2022
Supporting new moms in the postpartum period
By reaching out early and providing care that’s personalized to parents’ …

June 23, 2022
Collaborative care for serious mental health conditions
An innovative telehealth program gives patients direct access to pharmacists …

June 16, 2022
Leadership and innovation to prevent gun injuries and deaths
Kaiser Permanente’s new Center for Gun Violence Research and Education …

May 25, 2022
Be a source of comfort and calm
Trusted conversations help youth feel safe when community violence occurs.

May 3, 2022
One pill can kill: Understanding the risks of fentanyl
As overdose deaths skyrocket, an addiction medicine specialist explains …
March 30, 2022
A transgender man’s journey to become himself
A Kaiser Permanente member receives physical and emotional support from …

March 4, 2022
Online quiz helps predict likelihood of teen substance use
Assessment helps parents and caregivers intervene early when kids are at …

August 13, 2021
Remote patient monitoring improves care for chronic disease
If you have a chronic condition such as high blood pressure or diabetes, …

June 8, 2021
Cancer patients and physicians embrace telehealth
Video visits and virtual collaboration speed cancer care transformation …

May 24, 2021
Supporting access to telehealth for vulnerable populations
Kaiser Permanente grants help fund community organizations working to expand …
April 1, 2021
Campaign strives for equitable COVID-19 protection
The goal is to fill information gaps for COVID-19 prevention and vaccines, …

January 15, 2021
The fastest path to care
Available 24/7 with no appointment, e-visits offer Kaiser Permanente members …

October 2, 2020
Making (virtual) house calls
With expanded telehealth options, Kaiser Permanente members get convenient …

July 31, 2020
Telehealth
Expanding telehealth access

July 21, 2020
Transcending language barriers in health care for decades
Good communication is key to good health. During Kaiser Permanente’s 75th …

July 1, 2020
A breakout moment for virtual care
Kaiser Permanente’s fully integrated telehealth capabilities place quality …