News
Updates on everything that is Kaiser Permanente.
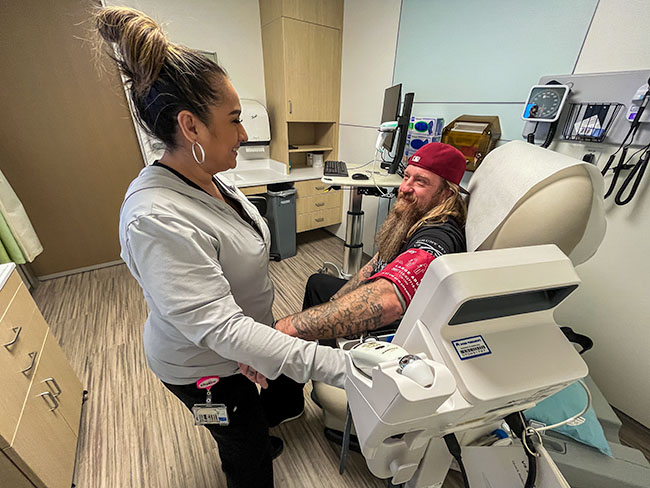
Welcome, Nevada
Kaiser Permanente and Renown Health joint venture clears the way for expanded access to affordable, high-quality care in 2027.
Latest press releases
February 9, 2026
Kaiser Permanente names Mike Bowers president of Northern California Region
February 6, 2026Kaiser Permanente and Risant Health report 2025 financial results
February 5, 2026Kaiser Permanente and RAJ Sports set new standard in care for elite women athletes
February 3, 2026Kaiser Permanente and Renown Health complete joint venture to serve northern Nevada
January 29, 2026Kaiser Permanente starts construction on new oncology wing
January 15, 2026Beth Leonard to join Kaiser Permanente as SVP and chief public affairs officer
January 13, 2026New, sustainably built Lakewood Medical Offices to open
December 22, 2025‘A Better Idea for Health Care’ is Kaiser Permanente’s 2026 Rose Parade® float theme
December 8, 2025Carrie Owen Plietz named group senior vice president, chief operating officer, Care Delivery
November 19, 2025Strengthening food security across the islands
November 14, 2025$50,000 grant for homeless and at-risk veterans
October 20, 2025Kaiser Permanente health plans earn high 2026 Medicare Star Ratings
October 7, 2025Moanalua Medical Center celebrates 40 years of excellence in health care
September 16, 2025Kaiser Permanente among nation’s best for treatment, prevention, patient experiences
September 10, 2025Kaiser Permanente launches in Nevada in 2026
September 9, 2025Craig T. Albanese, MD, to join Kaiser Permanente as President, Integrated Care and Coverage
August 20, 2025Jeff Krawcek, MD, named EVP and CEO for the KP Medical Foundation
August 15, 2025Nationally recognized for high-quality cardiovascular care
July 29, 2025Local teens join Neighbor Island Medical Scholars Program
July 29, 2025Kaiser Permanente hospitals named among best in nation
July 9, 2025Paul Minardi, MD, named EVP, Enterprise Clinical Integration and Growth
July 8, 2025Parker opening kicks off Kaiser Permanente’s new chapter in Colorado
July 7, 2025First Kaiser Permanente babies born at HCA HealthONE Rose
June 18, 2025Kaiser Permanente names Cynthia Dold president of Washington market
June 3, 2025Kaiser Permanente opens new expansion at Everett Medical Center
May 27, 2025Celebrating Project SEARCH graduates at Moanalua Medical Center
May 14, 2025Moanalua Medical Center on Newsweek’s Best Maternity Hospitals list
May 13, 2025Kaiser Permanente expands health care access in Coweta County
April 29, 2025Maui students gain hands-on skills at Career Exploration Day
April 24, 2025Neil Cowles named chief information and technology officer
April 17, 2025Pioneering renewable energy solutions
March 31, 2025Kaiser Permanente announces new hospital tower at its Sunnyside Medical Center
March 18, 2025Lahaina Clinic staff honored for volunteerism
February 17, 2025Sunnyside Medical Center receives Cardiac Surgery Award
February 7, 2025Kaiser Foundation Health Plan & Hospitals, Risant Health report 2024 financial results
February 4, 2025Shari Hofer joins Kaiser Foundation Health Plan of Washington board of directors
January 21, 2025Kaiser Permanente names Wendy Watson president for Northwest Region
January 17, 2025Kaiser Permanente names Corwin N. Harper president of Georgia Region
January 1, 2025Kaiser Permanente’s 2025 Rose Parade® float wins Wrigley Legacy Award
December 18, 20242025 Rose Parade float participants include Special Olympics athletes
December 16, 2024$125,000 in grants fight food insecurity among seniors
December 11, 2024Kaiser Permanente Portland hospitals named Best Hospitals for Maternity Care
December 3, 2024Risant Health closes Cone Health transaction, adds second health system in nine months
November 20, 2024The 2025 Rose Parade® float theme is ‘More Healthy Days for More Healthy Years’
November 12, 2024Kaiser Permanente named highest-rated Medicare health plan in Hawaii
October 23, 2024Kaiser Permanente partners with Atlanta Hawks to promote health and wellness
October 14, 20242025 Medicare Star Ratings: Kaiser Permanente health plans highly rated by CMS
October 7, 2024Expanding our relationship with HCA HealthONE in Colorado
September 16, 2024National quality report: Kaiser Permanente plans rated highest in all regions served
September 10, 2024Announcing a new strategic relationship with CommonSpirit Health
More from Kaiser Permanente
Kaiser Permanente Home